Health
Fentanyl kills in 45 seconds
Fentanyl and deadlier Carfentanil cut into crystal meth and cocaine
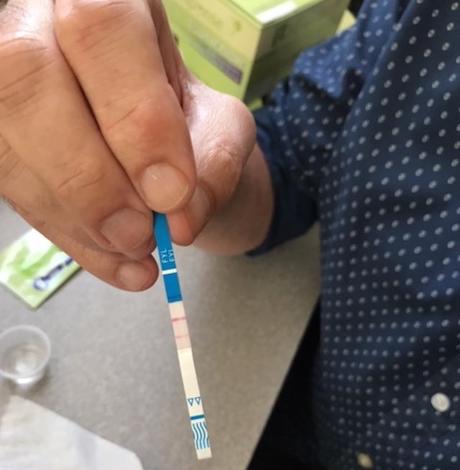
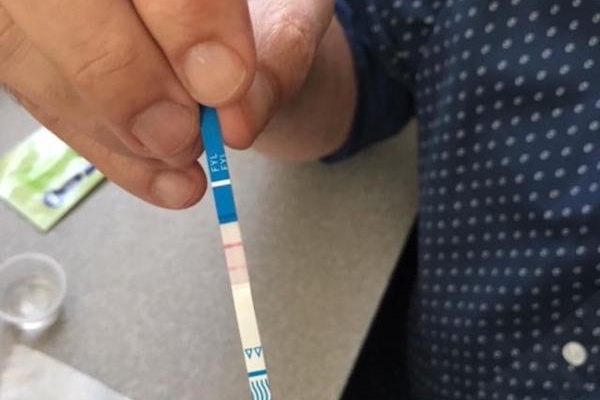
Los Angeles LGBT Center Addiction Recovery specialist Mike Rizzo tests a Fentanyl test strip. (Photo courtesy Rizzo)
Last month, the Palm Springs LGBT community experienced a surge of fear after two people were shot at the Toucans Tiki Lounge, a popular gay nightclub. Instantly thoughts went to the Pulse Nightclub massacre in Orlando, Fla., on June 12, 2016. Nerves calmed when the facts emerged, with Palm Springs Police Lt. William Hutchinson telling the Los Angeles Blade that the shooting is not being investigated as a hate crime.
That terrorist attack on the Pulse Nightclub left a psychic mark with LGBT people now being more vigilant, sometimes curtailing freedom for the sake of safety. But there are also moments and events where the old gay liberation culture clamors to let it all hang out, let gay Pride and freedom ring and party until the spirit says please, no more.
One such event is the annual White Party in Palm Springs, this April 26-29 celebrating its 30th anniversary of unbridled gay hedonism. But there may be a silent killer stalking the White Party for which the organizers and partygoers are unprepared —Fentanyl and Carfentinal, about which the Drug Enforcement Agency just issued a dire warning after three deaths in San Diego.
Fentanyl is usually linked with the nation’s ongoing opioid epidemic, which kills 130 Americans every day, according to the Centers for Disease Control and Prevention and for which opioid manufacturers are facing over 1,700 federal lawsuits, according to ABC News. Federal prosecutors are also looking at pharmaceutical executives and companies’ failure to properly report “thousands of suspicious orders of oxycodone, fentanyl and other controlled substances” to the DEA.
But the casual drug user attending the White Party or any other social gathering might not equate fentanyl in oxycodone with fentanyl in crystal meth, cocaine or other non-prescription drugs popular in the LGBT community. And that makes these new powder-forms even deadlier because one’s guard is down.
Mike Rizzo, manager of Addiction Recovery Services at the Los Angeles LGBT Center, only became aware of the deadly encroaching crisis last year when an employee died of an accidental overdose of Fentanyl that was “cut” into the cocaine he was using.
“This beloved employee was not an addict,” Rizzo told the Los Angeles Blade. “He and a few of his buddies where celebrating a friend’s birthday. There were four of them that used that night—three of them died. The fourth individual woke up at 6 a.m., thought his friends were asleep, went home and felt sick. That prompted him to go the ER, which probably saved his life.”
When he read about the Center employee’s passing on Facebook, Rizzo says, “I was in shock. I immediately ran to the office and started to do some research and found that Fentanyl was being cut with meth, cocaine and ecstasy. It has been a problem on the East Coast and it’s just now hitting the West Coast. This is very concerning for me.”
The more research Rizzo did, the more afraid he became.
“Pride was right around the corner. What was going to happen to casual users who would choose to celebrate Pride with a bump of meth or cocaine? An unsuspecting individual may lose their life because they wanted to have a good time,” Rizzo says. “Just because someone chooses to party doesn’t mean they should lose their life.”
Rizzo says there are five points to know about Fentanyl:
- Fentanyl can be 100 times more potent than heroin;
- Individuals may not know that what they are about to use may contain Fentanyl;
- The intervention rate for a heroin overdose is 1-3 hours; the intervention for a Fentanyl overdose is 45 seconds;
- The normal dose of Narcan may not be enough to prevent an overdose from Fentanyl, more may be needed;
- Of the meth samples tested in San Francisco, 78 percent tested positive for Fentanyl and 68 percent of the cocaine samples also tested positive for Fentanyl.
“One of the scariest parts of this,” Rizzo says, “is that people who are using meth or cocaine think they are using a stimulant and will not have the tools they need, like Narcan,” a nasal spray or Naloxone, an injectable (needle) solution.
Fentanyl is a cheap, apparently relatively easy to make synthetic drug that has become popular among drug dealers because it’s also highly addictive, as well as deadly when not dosed properly as in a legitimate prescription. Fentanyl can cause respiratory distress and death when taken in high doses or when combined with other substances, especially alcohol.
One example is the high-profile case of singer Demi Lovato, who was rushed to Cedars Sinai Medical Center last July after she was found unresponsive in her Hollywood Hills home. LACFD paramedics administered Narcan to the then 25-year-old pop star, reviving her prior to transport. It was believed at the time that she had ODed on oxy that may have been laced with Fentanyl.
As a drug 80 to 100 times more potent than heroin, Fentanyl may be classified as a weapon of mass destruction. “Fentanyl’s high toxicity and increasing availability are attractive to threat actors seeking non-conventional materials for a chemical weapons attack,” Assistant Secretary James F. McDonnell, Department of Homeland Security, wrote in a Feb. 22, 2019 internal memo to senior DHS and Defense Department officials asking them to consider classifying Fentanyl as a weapon of mass destruction.
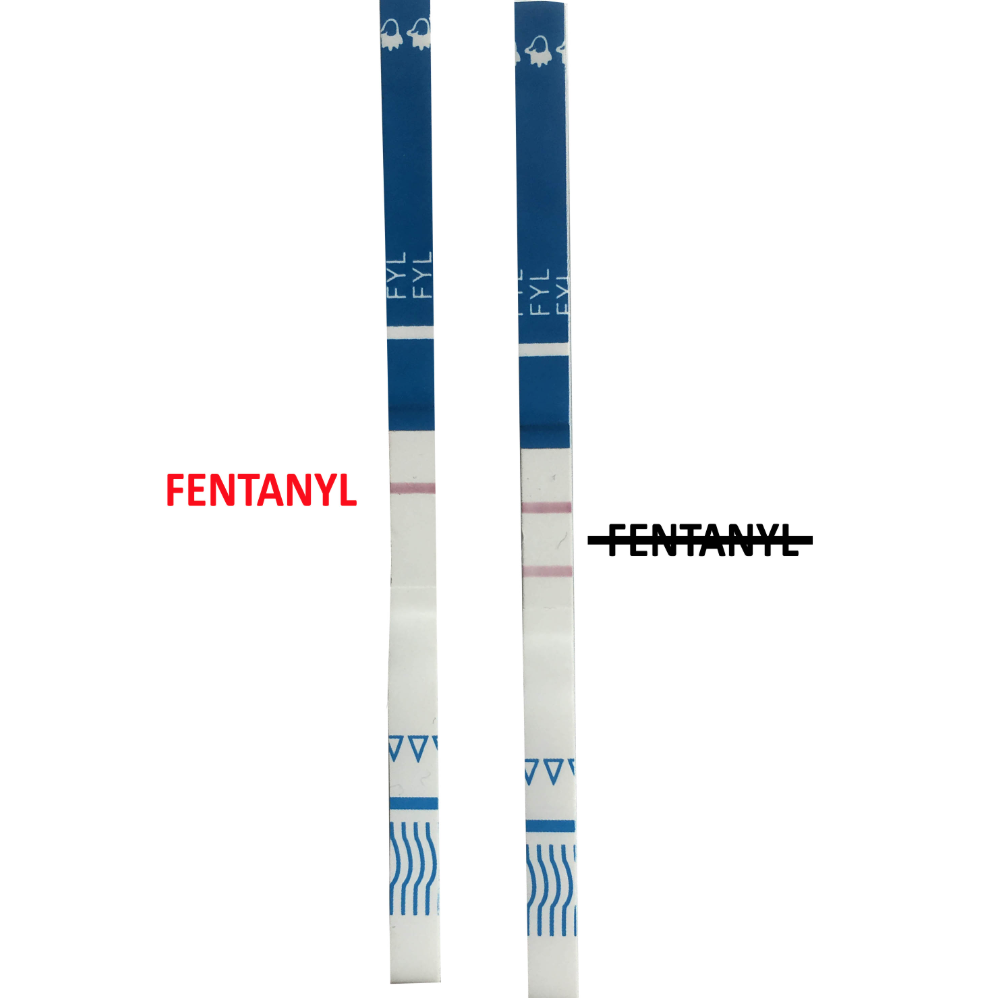
Fentanyl test strip (image from dancesafe.org)
In Nov. 2018, DEA Acting Administrator Uttam Dhillon announced results of the National Drug Threat Assessment that outlined the threats posed to the U.S. by domestic and international drug trafficking and the abuse of illicit drugs.
“Of all opioids, the abuse of illicit fentanyl and other synthetic opioids has led to the greatest number of deaths in the United States,” the report said. “Fentanyl is increasingly available in the form of counterfeit prescription pills marketed for illicit street sales, and also sold by traffickers on its own, without the presence of other drugs.”
On March 29, the editorial board of the Los Angeles Times took aim at the Trump administration’s diverting billions of dollars away from the opioid crisis.
“In 2017, the most recent year for which we have good data, more than 70,000 Americans died from drug overdoses,” The Times wrote. “Nearly 50,000 of those deaths involved opioids. New government data released this month show that a key driver of the overdose deaths in the last few years has been the spread of fentanyl, a synthetic opioid that has been mixed in with heroin and other illicit drugs. Extraordinarily potent, fentanyl is killing unwitting users in rapidly growing numbers.”
This prompted the West Hollywood City Council to vote on April 15 to proactively engage in “harm reduction” by making available Fentanyl test strips available to combat the problem.
“It’s important to target the casual user, as well as the addicts,” West Hollywood City Councilmember John Duran tells the Los Angeles Blade. “In the 1980s, I was legal counsel to Clean Needles Now, part of the efforts by ACT UP/LA to help in the prevention of spreading HIV.”
Harm Reduction is “a much needed step in to addressing these deaths caused by Fentanyl-related overdoses,” he added.
“We are doing this because WeHo is a hub for the LGBTQ community. This is a real public health emergency that has significant impact on the 40% of our population who are LGBT,” he said.
“People who are using—whether at a party or an event like the upcoming White Party or hook-ups on Grindr or other social events. They’re not expecting to use and then die,” Duran says. “We need to inform people as to the real dangers. They need to understand that even their casual party use can be lethal.”
Rizzo concurs. “With a 45-second intervention rate, the only defense is to test the product before you use it.”
Fentanyl Test Strips are available in every Center department and in all satellite locations, including Center WEHO. The City of WeHo recently gave the Center a grant for more test strips and this year the Center will do outreach at every Pride event. “We would like people to stock up before they attend these events and have them available for themselves or for friends who may choose to party,” Rizzo says. “If you do choose to party…party safer.”
Even deadlier than Fentanyl is carfentanil, one hit of the drug the size of a speck of dust can kill, the DEA reports.
“The DEA in San Diego County has issued an alert after three people have suffered documented fatal overdoses from a new form of the drug Fentanyl know as carfentanil,” CBS13 in Sacramento reported April 16. “It would only take 2 mg of the drug to cause a deadly overdose. Meanwhile, it would only take .02 mg of carfentanil to have the same fatal results.”
This synthetic drug is so fast-acting it not only attacks the brain stem to interrupt breathing but also rapidly closes the esophagus so even Narcon might fail to act in time.
The bottom line: freedom-loving gay partiers these days must become as vigilant about their drugs as they are about scoping out the exits at a crowded gay bar.
For more information about Fentanyl and the addiction services offered at the Center, please call 323-993-7448.
Viewpoint
I’m a queer Iranian Jew. Why I stand with Israel during this conflict
‘Hands Off Iran’ movement is erasure, not solidarity

The sirens cut through the night, jolting me from sleep. My heart pounds as I lie in bed, listening to the explosions outside. I don’t have to run — my Airbnb bedroom is a “mamad,” a reinforced bomb shelter built into the apartment. Though the windows are sealed, I can feel the building shake with each blast. This is my reality now.
I arrived in Tel Aviv just before the escalation with a delegation of North American LGBTQ leaders. We came to stand in solidarity with Israel’s LGBTQ community, which has increasingly been isolated by the global queer movement. After the delegation’s five-day mission, I had planned to stay an extra week. But on my first night here, the war broke out.
Despite the fear and chaos, I’m proud to be here. While I’m not a permanent resident of Israel — I live in Los Angeles, home to the largest Iranian Jewish community in the U.S. — I feel like I’m exactly where I’m meant to be. I work in both Iranian and Jewish advocacy spaces, and being here during this pivotal moment is an act of presence, of witness, and of resistance.
The adrenaline of seeing Israel strike back against the IRGC gave way to the sobering realization: I am in a war zone. But I know I’m safer here than I would be in many other places — because Israel protects its people. With shelters. With missile interceptors. With warnings. With a government that values civilian life.
In Iran, people don’t have that. The regime in Iran — and I use that term deliberately, because the regime is not the people — cut off internet access to prevent civilians from receiving IDF warnings before strikes. They wanted maximum casualties. They wanted suffering. They wanted images to manipulate. The same regime that imprisons, tortures, and executes LGBTQ people. The same regime that stripped my family, and millions of others, of their home.
So, when I heard the same anti-Israel activists who have spent the past 20 months calling to “globalize the Intifada” — a clear genocidal chant — adopt the new catchphrase “Hands Off Iran,” my heart sank. This is not solidarity — it’s erasure. These people defend the very regime that forced my parents to flee, tearing our family apart.
Romanticizing the Iranian regime with protest signs and slogans isn’t just tone-deaf. It’s prioritizing aesthetics over truth, trend over substance, and optics over people. It’s especially painful when I see it coming from my LGBTQ peers.
Growing up queer in the Iranian Jewish community during the ’80s and ’90s wasn’t easy. It was LGBTQ spaces that taught me how to stand tall in my truth — how to live authentically and reject shame. But now, those same spaces often turn their backs on me because I’m a Zionist, a widely misunderstood movement which simply calls for Jewish self-determination.
The hypocrisy of the current anti-Israel rhetoric is glaring. The “Hands Off Iran” movement is misguided, providing cover for a regime that tortures its citizens. Yet these activists were nowhere to be found during critical moments like the 2022 “Woman, Life, Freedom” uprisings, when Iranian women risked their lives burning their hijabs in protest. After Mahsa Amini was murdered simply for showing a little hair, those cheering “queers for Palestine” said nothing. This silence in the face of tyranny is not progressive — it’s dangerous.
For me, this conflict is not theoretical — it’s personal. I’ve witnessed firsthand how the Iranian regime targets LGBTQ people, religious minorities, and women. In Israel, I’m free to be who I am — a queer Iranian Jew. If we fail to stand with Israel, we fail to protect the values of freedom, human rights, and dignity. Israel is more than just a country — it’s a refuge for people like me, and it must remain that way.
As I write this, a fragile ceasefire is in place. But even with the quiet, the clarity remains. Israel is more than just a nation. It’s a refuge. And it’s worth standing up for — not because it’s flawless, but because it’s real. And because without it, people like me — queer, Iranian, Jewish — would have nowhere to turn.
Matthew Nouriel is a digital producer at the Tel Aviv Institute, Community Engagement Director at JIMENA, and a queer Iranian Jewish activist. He lives in Los Angeles.
Health
APLA opens eighth location in LA County
The WeHo location is named after Dr. Michael Gottlieb, the groundbreaking physician and researcher who in 1981 co-authored the first medical report identifying AIDS

The Michael Gottlieb Health Center is latest APLA facility to open, making it the eighth location in L.A. County to offer accessible healthcare services.
APLA Health recently opened its brand new the Michael Gottlieb Health Center in West Hollywood with a glitzy ribbon-cutting featuring a bevy of local politicians and community leaders on Friday, June 13. The new location, APLA’ eighth facility, will help the organization provide dedicated LGBTQ-inclusive health services to its more than 22,000 patients.
The new health center boasts 10 exam rooms offering primary, HIV and sexual health care, as well as mental health services. It also includes APLA’s first pharmacy and headquarters for the Alliance for Housing and Healing.
The WeHo location is named after Dr. Michael Gottlieb, the groundbreaking physician and
researcher who in 1981 co-authored the first medical report identifying the illness that
would later become known as AIDS. He later spearheaded important research on the
progression and treatment of HIV/AIDS and co-founded the American Foundation for
AIDS Research. He spent the last four years of his career at APLA, retiring in 2023.
“I’m honored to help dedicate this health center with my name on it,” Gottlieb told a
packed audience in the new center’s waiting room. “The center is named for someone
who is not of the community, but I’m proud to have my name up there, and grateful for a
community that has confided in me and trusted in me for decades now, and I continue
to stand with you in these difficult times in all the issues you’re facing.”
All of the speakers at the opening ceremony noted the difficult political climate for queer
people, immigrants, and health care under the new Trump administration in Washington.
APLA has already been forced to lay off its PrEP Navigation Team from its
Baldwin Hills location, as the federal government has terminated all contracts on HIV
and STD prevention with providers in LA County.
West Hollywood Mayor Chelsea Byers says this moment is an opportunity for the
community to come together to build a strong response.
“We have this opportunity to understand what we are able to do as a local community
against the backdrop of an administration like you had in the 80s,” said Byers. “I wasn’t totally there that whole time. But this link between past experience and present moment is really critical. It’s heartening to see so many community leaders. It’s a really amazing moment we have as a community. At a time when care is needed to be extended to more than ever
before I’m grateful to APLA for making such a beautiful space where care can shine so
bright in our city.”
U.S. Rep. Laura Friedman (CA-30) agreed with that sentiment.
“We have seen this administration deliberately demonize members of our community.
They have demonized immigrants, minorities, our trans community members. They’ve
turned their back on the LGBT community, cruelly cutting funding for AIDS prevention
and STDs. And yet, coming into West Hollywood and this community, and into this
room, we see there’s a tremendous amount of caring and love,” said Friedman. “That is
how we change things in this country, by living those values every day.”
“At a time when the federal government is no longer a partner in anything medical, this
facility is going to provide an incredible and needed safety net for patients,” she said.
Despite these threats, APLA Health CEO Craig Thompson says the organization is
committed to serving everyone who needs care.
“The need for people for health care is going to continue regardless of what the federal
government does around funding, and we’re committed to being there to provide that
health care in all the different ways we possibly can,” he says.
One of the new ways APLA’s new facility will improve service to its patients is through
its new in-house pharmacy.
In addition to fostering closer connection between a patient’s doctor and pharmacist, APLA will offer free delivery at no charge to patients and will help consolidate prescriptions to make it easier for patients to receive and take their medicine.
“We’ve been wanting to close the loop on comprehensive care and offer a pharmacy for
our patients, that way they can get all the support withing one organization,” says Rich
Kowalski, APLA director of pharmacy.
Opinions
Pride and Protests: A weekend full of division
Amid more upcoming raids and protests, we will have to learn when to act, how to react and when to find pockets of joy to celebrate in, because those moments are also acts of resistance

While many Angelenos celebrated the 55th annual L.A. Pride and mainstream news outlets like ABC7 and FOX11 news covered the celebrations, the reality for many other Angelenos involved tear gas, rubber bullets and breaking news coverage from community-led outlets like CALÓ News.
If we were to take a step back into the history of Pride, we would be angered by the amount of violence and pain that led to the protests on the dawn of June 28, 1969. The Stonewall uprising took place as a result of police raids at the now-infamous Stonewall Inn on Christopher Street in New York City. The night that has gone down in history as a canon event for queer and trans life began when police raided the Stonewall Inn and arrested multiple people. The arrests and the police brutality involved, led to an uprising that lasted a total of six days.
Marsha P. Johnson and Sylvia Rivera were credited as being the first people in that historical moment to start the movement we now know and celebrate as Pride. They were Black and brown, people who transformed our notions of fear and action, modeling the mantra that we must act in order to not live in fear. The people at the Stonewall Inn on that night in June all those years ago, and all of the queer and trans people now, have something deeply unsettling in common.
We both live in a constant state of fear and anxiety.
We live in such a major state of fear that anxiety, depression and other mental health issues — including substance abuse disorders — tend to be particularly prevalent in the LGBTQ community. According to Mass Gen, the U.S. is facing a mental health crisis, with nearly 40% of the LGBTQ population in the U.S. reported experiencing mental illness last year, a figure of around 5.8 million people.
Pride began as the very type of protest that went on this past weekend over the U.S. Immigration Customs Enforcement (ICE) raids, where people have been taken into custody, reporters shot with rubber bullets and tear-gassed, and where union president David Huerta was taken into custody and charged with alleged federal conspiracy charges.
Over the weekend, I celebrated Pride. I admittedly celebrated being queer, while my other communities experienced fear in the face of arrests, tear gas to the eyes and baton blows to the head. It was an internal battle I was not prepared for and a real battle on the streets I was not ready to experience. It made me feel weak and more than anything, I felt tired. I felt scared and I felt like I was not prepared for what was to come from these arrests and this violence.
I am a proud child of immigrants. My mother is Colombian and migrated here in the early 80s, settling down in West L.A and building a life with children, houses and her religious community.
My father migrated here in the mid-to-late 80’s from Mexico, where he and his family were hardworking farmers. He has worked at his job, without rest, for over 35 years. He rose up the ranks from line worker to general manager. He does not miss work. He follows every rule and he is never late. Both are documented, but only because of luck and the ease of getting papers back when there weren’t so many bureaucratic steps to gaining citizenship or a green card legally.
My parents and their extended family are proof of a now-distant American Dream, one in which we gain status, we become homeowners and business owners, have children and send them off to college to learn things that our parents can’t even imagine.
Though they did the best they could, my parents had other challenges and barriers to their success. So I worked hard in order to succeed for them. I did it for all of the people in my communities. I did it to raise the statistics on Latinx people, LGBTQ people and former foster youth who go on to college despite the odds and get higher education degrees.
My road to where I am now was paved with uncertainty, food insecurity, homelessness and many other factors that pushed and pulled me back. The analogy I can think of to accurately compare myself to is a catapult. I was pulled down with weights that were added on more and more, until one day I catapulted forward into the life I now have the privilege to live. Though I still struggle in many ways, it is the first time in my life that I am not in survival mode. It’s the first time in my life that I get to exist as a queer person who can enjoy life, build a friend group and establish deep connections with people. It’s also the first time I get to enjoy Pride as someone who is single and who has spent the past 18 months healing from my from my last relationship.
It was the first time in my life, as a lesbian who’s been out for over a decade, that I truly planned to enjoy Pride with my groups of friends.
While I was there this weekend, my internal battle began and I felt torn between celebrating my life and my queerness and covering the ICE raid protests happening not too far from Sunset Blvd.
What I didn’t expect was to see so many other people at Pride, completely oblivious and completely disconnected from the history of Pride, instead glorifying corporate brands and companies that have remained silent over LGBTQ issues, while others have gone as far as rolling back their Diversity, Equity and Inclusion initiatives.
If Marsha P. Johnson or Sylvia Rivera were there at that moment, they would have convinced us to merge our Pride celebration with the protests. They would have rallied us all to join forces, and in the spirit of Pride, we would have marched for our immigrant community members, fighting for their right to due process.
I’m not sure if I made the right decision or not, but the next 60 days will say a lot about every single one of us. We will have to learn when to act, how to react and when to find pockets of joy to celebrate in, because those moments are also acts of resistance.
The Trump administration vowed to strip away rights and has made it their mission to incite violence, fear and anxiety among all working class, BIPOC and LGBTQ people, so it is important, now more than ever, to unite and show up for each other, whether you’re at a Pride celebration or a protest.
The next 60 days will raise our anxiety and fear, but we must remember to also take breaks, celebrate wins, relish in community, hug your loved ones and use whatever amount of privilege that you have, to show up for the communities that are hurting the most in these moments.
Juneteenth is also coming up soon and I hope to see more of us rally around our Black brothers, sisters and siblings, to not only fight for our rights, but to continue celebrating ourselves and each other.
In the words of Marsha P. Johnson: “There is no pride for some of us, without liberation for all of us.”
California
New California trans athlete policy creating ‘co-winners’ is a crock
You didn’t misread that. Hernandez shared the podium with ‘co-winners’

A lot happened at last weekend’s high school state track and field championship meet in
Clovis, Calif. Parents of cisgender student-athletes booed the one and only transgender
girl competing. Police and security officers showed up in large numbers to keep
protestors apart and safeguard the competitors. Police made an arrest outside the
stadium after a demonstrator brandishing a transgender pride flag allegedly assaulted a
man described as a conservative activist and caused damage to his vehicle.
The trans student — 16-year-old AB Hernandez — finished a winner. But she wasn’t “the” winner.
As CBS News reported, “Hernandez took home first place medals in both high jump and
triple jump and she placed second in the long jump event. Following a rule change by
the California Interscholastic Federation, a co-winner was named in each of the three
events in which Hernandez placed.”
You didn’t misread that. Hernandez shared the podium with “co-winners.”
As the Blade reported last week, the CIF introduced a new “pilot entry process” that for
the first time, allowed judges to score trans athletes separately from cisgender
competitors, so there were three winners in every event: a cisgender male winner, a
cisgender female winner and a trans student-athlete winner.
The new policy was announced hours after President Donald Trump threatened to pull
“large scale federal funding” from the state if officials allowed trans athletes to compete
according to their gender identity.
Despite the policy change, the U.S. Department of Justice announced on social
media it was investigating State Attorney General Rob Bonta, State Superintendent of
Public Instruction Tony Thurmond, the Jurupa Unified School District, and the CIF for
potential violations of Title IX, as the Blade reported.
So what happens now? As KXTV reported, President Trump issued another threat to
pull funding on Monday in a post to his Truth Social account, not naming Hernandez but
labeling her “a biological male” and using his favorite derogatory nickname for
California’s Democratic Gov. Gavin Newsom.
“A Biological Male competed in California Girls State Finals, WINNING BIG, despite the
fact that they were warned by me not to do so. As Governor Gavin Newscum fully
understands, large scale fines will be imposed!!!”
Now, the pundits are weighing-in. Sara Pequeño wrote in USA Today how she was
encouraged to see Hernandez share the 2nd place podium with Brooke White and “put
their arms around each other.”
“They’re setting an example for how all of us should treat our trans neighbors, i.e.,
treating them like human beings, not enemies,” she wrote.
As Pequeño noted, Save Women’s Sports, an anti-trans advocacy group, could only
identify five trans students in the entire United States who were competing on girls’
teams from kindergarten through grade 12 in 2023. “That group’s entire existence is to
hate trans athletes, and they found very little to hate,” she wrote.
According to the president of the NCAA, there are fewer than 10 student-athletes
who publicly identify as transgender out of the more than 500,000 competing at the
collegiate level.
Pequeño was not alone in finding joy in the rules change that brought cisgender and
transgender girls together on a podium, each of them a “co-winner.” So did self-
proclaimed “trans advocate” Cyd Zeigler.
He’s one of the co-founders of the LGBTQ+ sports site Outsports, who in 2023
infamously came close to endorsing Florida Republican Gov. Ron DeSantis for
president, only to offer his regrets, following a backlash from readers. Zeigler penned an
op-ed Wednesday originally titled “California trans athlete policy is something everyone
can embrace.”
“Everyone?” Not this sports editor.
He called the new CIF policy “the best possible path in 2025 to trans participation in
sports.”
In celebrating this change, Zeigler also trashed “goal-post-moving trans advocates” and
policies in California and Connecticut that allow “a trans girl to run in boys track meets
and, without a medical transition, later compete in girls meets,” meaning high school
competitions. “That’s bad policy,” declared Zeigler without evidence.
That policy in Connecticut has stood since 2011 and is enshrined in state law, and so far
has withstood legal challenges once again being heard in federal court.
Outsports at some point changed the headline of his screed to “New California trans
athlete policy is something we can embrace” and apparently made another significant
choice: Despite quoting the outlet’s one and only remaining transgender contributor,
Karleigh Webb, who opposes the rules change, Zeigler did not mention her by name.
Why?
In an article published before the championship, Webb wrote: “If AB Hernandez wins,
why should she have to share the spoils with someone else if’s not a tie? That’s what
professional transphobes like Jennifer Sey and Riley Gaines try to sell. Awarding a
duplicate medal gives their nonsense credence to the detriment of the sport and the
athletes.”
Webb is right. Zeigler and the CIF and Gov. Newsom are wrong. You either win, or you
lose, or if you prefer, you come in second, third, whatever. But “co-winners?”
That’s a crock.
Imagine if the Dodgers and Yankees shared the World Series trophy. Why shouldn’t the
49ers also win the Super Bowl alongside the Chiefs? Maybe Kamala Harris should be
declared a “co-winner” of last November’s election?
Personally, I’m glad to see Hernandez embraced by her cisgender peers. I’m relieved to
know that crowds cheering these amazing girls last weekend drowned out the hecklers
who showed up to boo a child. I’m encouraged that even if she had to share the win,
Hernandez was given her rightful place among the teens competing and proved she
was not only worthy of competing but did not win in every event.
So, she’s hardly “unbeatable.” Most trans athletes actually lose, as Zeigler wrote almost
six years ago, back before he started echoing anti-trans inclusion activists Martina Navratilova, Renee Richards and Nancy Hogshead-Makar.
If he really thinks the CIF “co-winners” rule is going to silence anti-trans forces, I think
he’s going to be very surprised by Riley Gaines and her crowd.
While it’s easy for Zeigler to concede public opinion has shifted, he should know
better than to blame those who pushed for inclusion, when it’s clear that conservative
voices in media and politicians, like his, are the ones responsible for influencing that
move to reject trans women’s right to compete in women’s sports. It’s a pendulum swing
that in time will undoubtedly swing back, once the science proves that trans women and
girls don’t always win. In fact, researchers have already proven some trans athletes are
at a disadvantage compared to their cisgender competitors.
Just as Parker Molloy reported that a Republican-commissioned study on gender
affirming care in Utah actually found “that youth who received care before age 18 had
better outcomes, especially around depression, anxiety and suicidality. Hormonal
treatments were associated with positive mental health and psychosocial functioning
outcomes.”
I believe the science is on the side of transgender Americans. Americans love a
winner. Not a “co-winner.”
Opinions
Trump’s inhumanity won’t erase Andry Hernandez Romero, if we resist
Andry Hernández Romero’s case continues to be a violent reminder that we must rise up and resist

Editor’s Note: Since this article was first published, more information on Andry’s case has become available.
UPDATE: On June 4, a federal judge ruled in favor of the ACLU and Democracy Forward in J.G.G. v. Trump, in which deported gay stylist Andry José Hernández Romero is one of the lead plaintiffs. Describing the Venezuelan deportees’ situation as Kafkaesque, Judge James E. Boasberg said the plaintiffs would likely prevail in their complaint about being denied due process, the New York Times reported. Trump officials, Boasberg wrote in his 69-page ruling, “spirited away planeloads of people before any such challenge could be made. And now, significant evidence has come to light indicating that many of those currently entombed in CECOT have no connection to the gang and thus languish in a foreign prison on flimsy, even frivolous, accusations.”
“Absent this relief,” the judge wrote, “the government could snatch anyone off the street, turn him over to a foreign country and then effectively foreclose any corrective course of action.” He ordered the Trump administration to give the deportees the due process they have been denied.
On Friday, June 6, Rep. Pramila Jayapal (WA-07), Ranking Member of the Immigration Integrity, Security, and Enforcement Subcommittee, will host a shadow hearing Kidnapped and Disappeared: Trump’s Lawless Third Country Disappearances at which Andry’s attorney Lindsay Toczylowski will testify.
The juxtaposition is morally excruciating. The very air in West Hollywood is electric with
queer joy and the excitement of WeHo Pride, but it’s more than a celebration of our ongoing
movement for liberation and equality. We’ve been waiting for a moment to exhale and
stop the clamor of the Trump horror show.
What can we do to stop this overwhelming dictatorship campaign that is gleefully
enforcing Project 2025 through a deluge of cruel Executive Orders, demonizing and
erasing anything under Diversity, Equity and Inclusion initiatives and LGBTQ while dispatching masked ICE agents to snatch anyone Trump’s White Supremacist terrorist administration tags for deportation.
Among those swept up in Trump’s frenetic crusade is Andry Hernandez Romero, a 32-
year-old gay hair stylist and makeup artist who fled harassment and threats of violence in Venezuela in May 2024, after speaking out against authoritarian dictator Nicolás Maduro. After navigating the complex app designed to streamline the byzantine U.S. lawful entry process, last August Romero faced a U.S. border official in San Diego. With no criminal history, he demonstrated a “credible fear of persecution” to proceed with an asylum case.
Imagine what Romero felt — so close to freedom, to opportunity, to unabashed queer joy.
Then came that Trumpian twist.
During a physical exam, officials fixated on Romero tattoos of crowns with the words “Mom” and “Dad.” The agent apparently assumed that Venezuelan gangs accept gays because he suspected Andry had gang affiliations and does not fact check because Tren de Aragua does not use crown tattoos for gang identification.
Romero landed in detention awaiting his asylum court date. But one week before the
March 13 hearing in San Diego, Romero was abruptly transferred to a facility in South
Texas, resulting in his absence in court. The hearing was postponed to March 17 when
the immigration judge again asked where Romero was.
“He was removed to El Salvador….we just found out today,” the ICE lawyer replied. The judge questioned the legality of Romero’s deportation without a removal order.
On March 14, Trump invoked the Alien Enemies Act — a 1798 law used during a
declared war — to target immigrants as government “enemies” who had “infiltrated”
America. Secretly, ICE deported Romero and 137 other Venezuelans to El Salvador’s
notorious Terrorism Confinement Center, with Trump paying dictator President Nayib
Bukele to incarcerate the kidnapped immigrants.
The world watched as Andry and his shackled fellow prisoners were displayed on TV
brutally forced off the plane and forced to kneel as agents roughly shaved their heads.
TIME Magazine photographer Philip Holsinger reported that Romero was being slapped while crying out for his mother, “I’m not a gang member. I’m gay. I’m a stylist.”
Trump called the Venezuelans “rapists,” “savages,” “monsters” and “the worst of the
worst,” claiming they were thoroughly vetted. But ProPublica reviewed each case of the
Venezuelan deportees and reported that the Trump administration knew that “the vast
majority” of the 238 Venezuelan immigrants ”had not been convicted of crimes in the
United States before it labeled them as terrorists and deported them, according to U.S.
Department of Homeland Security data that has not been previously reported.”
Lee Gelernt, the American Civil Liberties Union’s lead attorney fighting the deportations,
told ProPublica that the removals amounted to a “’blatant violation of the most
fundamental due process principles” and subjected the deportees to life imprisonment.
There have been numerous attempts to look for a humanitarian bone in the Trump
administration’s body politic, most notably gay immigrant Rep. Robert Garcia’s heated
exchange with Homeland Security Secretary Kristi Noem during a May 14 congressional hearing. Garcia (D-Long Beach) went to El Salvador for a welfare check
but was denied access to Romero.
“He has had no access to lawyers or family since he has been taken over a month now,”
Garcia told Noem. “His mother just wants to know if he is alive.”
“I don’t know the specifics of this individual case. This individual is in El Salvador and
the appeal would be best made to the president and to the government of El Salvador
on this,” replied Noem.
Garcia pushed back.
“You and the president have the ability to check if Andry is alive and is
not being harmed. Would you commit to at least asking El Salvador if he is alive?”
Nope.
“This is a question that’s best asked to the president and government of El
Salvador,” she said.
Noem’s callous disregard for life and suffering is unsurprising. The former governor of
South Dakota blithely noted in her political memoir that she shot and killed her 14-
month-old dog Cricket when the puppy misbehaved. “I hated that dog,” Noem wrote.
She also shot a goat she didn’t like.
“In neither case did Noem show any doubt or remorse; quite the contrary, she sought to
cast her action as a signifier of tough-minded realism that would burnish her appeal as a
politician from a rural community,” wrote Sara Amundson, president of the Humane
Society Legislative Fund.
So if Noem thinks callousness is cool, imagine how she feels about someone she might
deem as sensetive?
“Under the Constitution, every single person has a right to due process, and that means
they have a right to notification of any allegations the government is making against
them and a right to go into court and prove that those allegations are wrong if that’s the
case,” Lindsay Toczylowski, President of the Los Angeles-based Immigrant Defenders
Law Center who is representing Romero pro bono, told NBC News San Diego April 11.
“In Andry’s case, the government never gave us that opportunity. In fact, they didn’t even
bring him to court, and they have forcefully sent him to El Salvador without ever giving
us any notice or without telling us the way that we could appeal their decision.”
On May 27, Immigration Judge Paula Dixon granted a U.S. Dept of Homeland Security motion to dismiss asylum proceedings for Romero scheduled for the following day.
“We should all be incredibly alarmed at what has happened in Andry’s case. The idea
that the government can disappear you because of your tattoos, and never even
give you a day in court, should send a chill down the spine of every American. If this can
happen to Andry, it can happen to any one of us,” said Toczylowski.
Andry’s life depends on us holding the Trump administration accountable for what they
have done to him,” Toczylowski said. “We will continue to fight until Andry is safe and
free.”
Romero is a lead plaintiff in the American Civil Liberties Union’s and Democracy Forward’s J.G.G. v. Trump case in which Romero’s friend and mother gave statements that are now evidence saying Romero “was persecuted both for his sexual orientation and for his refusal to promote government propaganda” while working as a makeup artist at the TV network in Caracas, according to CNN.
But Project 2025 booster Kevin D. Roberts doesn’t care, having ordered the Trump
administration to delete “the terms sexual orientation and gender identity….out of every
federal rule, agency regulation, contract, grant, regulation, and piece of legislation that
exists.”
So do Trumpland judges care about the raison d’etre for asylum or is that too DEI?
NBC News reported that Romero’s dismissal order “allowed for the possibility that the
case be reopened if Hernandez returns to the U.S.”
That’s why we the people, must rise up and resist.
“As the son and grandson of Japanese Americans who were rounded up and forced into
camps without due process, I know all too well that Andry is not the first person to be
unjustly taken by the government,” says out Rep. Mark Takano (CA-39), Chair of the Congressional Equality Caucus. “Every American should be alarmed by how openly the
Trump Administration is taking people off the street and locking them away in a foreign
prison without so much as a day in court — all because of their tattoos. This fight is not
over yet, but every day it drags on puts Andry and others’ lives in danger. I stand with
Andry, his family, his lawyers, and our Constitution in rebuking President Trump’s cruel
and illegal attacks, and hope that justice is swiftly served.”
Longtime activist Cleve Jones urges all LGBTQ people and allies to take action.
“We don’t know if he’s dead or alive,” Cleve says. “I look at [Romero] and he’s like my little
gay brother who is now in this terrible situation where he — if he is still alive — is probably
being subjected to horrendous brutality on a daily basis.”
But Cleve is also angry at the lack of response to this urgently important case.
“If you want to be intersectional and not just quack about it, look at this case,” Cleve
says. “This young man stands at the intersection of our fight for LGBT equality, for
immigrant rights, and for due process under law.”
San Francisco Pride and New York City Pride rejected his request to name Andry an
honorary Grand Marshal. But, Cleve says, “I’m happy that a number of pride
celebrations have done that. Others have stepped up and are organizing fundraisers. I
see there’s one coming up in New York. But everybody should be talking about Andre.
Free Andre. Free Andre. It’s so important!”
Please note: To support Romero’s case and others like it, the Immigrant Defenders Law Center is selling a T-shirt that says “Asylum is a Human Right, found here.“
Health
Brave, Not Broken: Mental health, queer identity and the urgent fight for care
As we near the end of Mental Health Awareness Month, Dr. Greg Cason shares what has changed, what is at risk and why therapy and community matter more than ever

Let’s get one thing straight (well, not too straight), mental health awareness is having its moment — and it’s about damn time.
For LGBTQ+ folks, mental health is not a trend. It is survival. In a time when therapy is finally making its way into casual brunch talk (please stop referring to drinking mimosas as “self-care”), and TikTok is where so many go to share their experiences, we sat down with a psychologist who’s been doing the work long before it was mainstream. Equal parts clinician, advocate and reality TV veteran, Greg Cason offers an authentic and insightful look at queer resilience, the dangerous return of bad policy and why healing often begins with three brave words: I need help.
What does this time signify for you both personally and professionally?
Personally, I am thrilled about how far we’ve come in de-stigmatizing mental health, especially in the LGBTQ community in my lifetime. Professionally, it’s a reminder that my job isn’t just in the therapy room, it’s also about education and advocacy. Social media has helped normalize mental health talk and organizations like National Alliance of Mental Health (NAMI), have been the backbone of that effort. It’s not perfect, but we’ve gone from whispers, to full-blown open dialogues and that’s powerful. But our work is not over.
The current administration in D.C. is taking apart decades of needed research, bringing back discrimination against our LGBTQ brothers and sisters and instituting a “health” agenda based on fringe theories as well as giving voice to influencers over experts. We’ve come a long way, but it’s fragile and if we don’t stand up to the current assaults, we will find ourselves back to the limitations and attitudes that prevailed before most of us were born.
This year’s theme, “Turn Awareness into Action,” emphasizes moving beyond recognition, to tangible change. How can people take meaningful steps to support and promote mental health?
For you personally: start small.
Check in on your friends — really check in. Advocate for better mental health policies at work or school. Normalize therapy. Share your own experiences and together we also need to act. We can’t fall for the constant demonization of members of our own and other communities. We must band together to stand up for the less fortunate and to push back against new assaults. If you truly want to improve your mental health, connect with your community.
What are some common mental health issues faced by queer folks and how does therapy address them?
Higher rates of anxiety, depression, substance use and trauma — much of it rooted in or exacerbated by rejection, discrimination, or internalized shame. Therapy helps untangle those experiences, identify core beliefs, and replace harmful narratives with empowering ones. It’s about rebuilding a sense of self that the world may have tried to tear down.
Even so, therapy is not the only solution. Don’t underestimate the power of community support groups such as Alcoholics Anonymous (AA) and similar organizations. These are powerful resources that not only help you with issues like substance abuse, but also help you to rebuild community and connection.
What’s one myth about queer mental health that you’d like to call out and nip in the bud?
That being LGBTQ causes mental health problems. That’s flat-out wrong. The issue isn’t our identities — it’s the way society treats us. Remove the stigma, support queer folks and the mental health gap shrinks dramatically. But an honorable mention for a rising tide of a disproven and harmful therapeutic approach called “Conversion Therapy.”
Though it promises to change sexual and gender orientation, the only thing it does is shame [LGBTQ people] into silence and produce further trauma. It’s sad when politics and religion drive health priorities without any consideration of science and human functioning.
As a practicing psychologist, how have you seen the conversation around mental health change and evolve, especially within our LGBTQ community?
It used to be shrouded in silence — now it’s becoming part of our culture. I see LGBTQ people openly discussing therapy, boundaries and healing in casual conversations. That’s revolutionary. But I cannot help but think it was born out of necessity.
When AIDS was first identified in 1981, the world also saw therapy as only for those who were mentally ill. But it became a necessity for our community. The ever-present fear of disease and dying was commonplace in our community, combined with the constant assaults from politicians, religious professionals, family, and even friends, we had to identify people that we could open-up to and seek support from.
Those were dark and difficult times and we have progressed in ways that seemed impossible back then. That shift is showing up in the language, the pride, and the resilience of our community.
Your particular practice focuses on Cognitive Behavioral Therapy (CBT). How does CBT serve as an effective tool in addressing mental health challenges in our LGBTQ communities?
I always have to laugh — (CBT) has a very different connotation in our community. But in my world, it stands for the more mundane psychotherapeutic modality. (CBT) is powerful because it helps people understand how their thoughts shape their feelings and behaviors.
That said, it also has a dark past. (CBT) techniques were once used in “Conversion Therapy” to try to change sexual orientation — which is now widely recognized as both unethical and harmful. Today’s (CBT) is different. It’s science-based, jargon-free and focused on helping people recognize and replace harmful beliefs shaped by family, religion, or society.
But it’s not just about thoughts. We also work on behavior change, emotional regulation and achieving goals. It may not sound sexy, but I’ve seen it transform individuals, couples and groups.
I was lucky to do a fellowship with Albert Ellis, one of (CBT’s) pioneers. He taught me two things I always keep close: First, we’re all fallible, fucked-up human beings — and that’s okay. Second, change takes work and practice.
And, as another mentor once said, “change may take a while… so pack a lunch.”
You once starred on Bravo’s LA Shrinks. Did your time in reality television provide you with any new perspectives on psychology or on yourself?
Oh absolutely. Being on “LA Shrinks” was both a wild ride and a mirror (albeit cracked, at times). It reminded me that therapists are human too — flawed, funny, and fully visible. It also deepened my empathy for clients in the public eye. Having your life edited for entertainment is… let’s just say, psychologically complex.
Reality television has become a significant portion of most entertainment and media these days. In what ways and to what scale do you believe it has impacted the mental health of our queer communities?
Reality TV is a double-edged sword. On one hand, it gives visibility to LGBTQ stories — sometimes for the first time. My husband and I were married on the show and that meant so much to me to share that reality with those kids out there like me who grew up without any gay role-models or any hope for a relationship or normal life. On the other, it can flatten people into caricatures. The audience forgets they’re watching a curated narrative — not a whole human being.
I have known some people who were portrayed in a certain way that did not capture their full character, and they suffered as a result. The danger lies in mistaking visibility for authenticity. Reality TV can inform, inspire, or exploit — and often does all three at once. Nonetheless, I cannot tell you how many people said they watch reality TV while they did other things like ironing or laundry. They said it was having their friends with them. That always made me smile.
As someone who’s both a therapist and a public figure, how do you personally stay grounded while continuing to hold space for others?
I have always believed that it is important to leave the therapist at the office. There are people in my profession that don’t allow themselves to be vulnerable in their relationships, silly with their friends, and thrilled to be home alone with a pint of ice-cream and a remote control. We are humans first. So am I. As for anyone approaching me because they saw me on TV or now listen to my podcast, I am always flattered. I realize they are offering me a gift. I don’t have to question the gift or tell them that it is not my size. Rather, my only job is to graciously accept. Doing that has only made my heart grow larger, not my ego.
What advice would you offer to encourage people who hesitate to seek help and begin their journey toward healing?
Therapy doesn’t mean you’re broken — it means you’re brave. Start with one conversation. One resource. One step. You don’t have to commit to a lifetime of therapy — just be open to the possibility that healing is available and that you deserve it.
Looking ahead, what changes or improvements would you like to see in mental health care for the LGBTQ community?
Access, affordability and cultural competency. We need more LGBTQ therapists — and more allies who understand our lived experiences. A personal desire of mine is that therapists focus on science rather than cultural trends or social media diagnoses and treatments. I know the era of social media is making everything a popularity contest. But I hope we can also not forgo expertise just to follow the latest fad.
Whether you’re starting therapy, advocating for others, or simply sharing your story — remember: awareness is only the beginning. Action creates change.
Community Perspectives
‘Protect the dolls’: The viral t-shirt that sparked a movement
The shirt’s message and its impact have turned this moment into a cultural flashpoint

In February 2025, American designer Conner Ives closed his fall and winter show at London Fashion Week with a striking message — not spoken, but worn.
He walked the runway in a T-shirt reading “Protect the Dolls” a phrase that has since gone viral and ignited a wave of support for trans rights around the world. The shirt, now worn by celebrities and activists alike, has become more than a fashion statement — it’s a declaration of solidarity, a tribute to trans dignity and trans rights and a call to action.
“The night before the show, my team and I were sitting around throwing around slogans that we would put on a shirt, which led to Protect the Dolls,” explained Conner Ives in an interview with Trans Lifeline.
The phrase, simple yet powerful, was designed to cut through the noise.
“Maybe the reason that the catchphrase caught on,” said Ives. “Is that rather than coming in with testimonials or facts or percentages… this was maybe a way to simplify down the message to something that could just be said in three words.”
The word “doll” has deep roots in LGBTQ culture, tracing back to the 60s and 70s ballroom scene created by Black and Latino, trans and queer communities. In a world that routinely rejected them, calling each other “doll” was an act of affirmation — a way to celebrate beauty, softness and survival. The term of endearment became a symbol of sisterhood and resistance — a coded language of care in hostile environments. By calling each other dolls, we affirm our beauty, our care and our worth. Like the way societies throughout human civilization have treated cherished dolls — with love, nurture, and tenderness — the term has become a powerful emblem of resistance, sisterhood and self-love.
Today, as trans rights face increasing attacks both in the U.S. and around the world, remembering this legacy feels more urgent than ever. Earlier this year, President Donald Trump, now in his second term, signed multiple executive orders severely restricting transgender rights. Meanwhile, in the U.K., the Supreme Court’s redefinition of “woman” has excluded trans women from key legal protections, marking a major setback for equality. As Ives reflected, “It feels like we are sometimes living in two alternate realities simultaneously… the alternate reality where we have the people that we choose around us, and then the one filled with political theater and hysteria.” In this climate, “Protect the Dolls” is more than a slogan — it’s a rallying cry to defend our rights, affirm our dignity and celebrate the communities we build together.
The shirt’s message and its impact have turned this moment into a cultural flashpoint. Celebrities across fashion, film, music, and social media have rallied around the design, turning their platforms into megaphones for its mission. Pedro Pascal wore it to his 50th birthday party alongside DJ Honey Dijon and again at the European premiere of “Thunderbolts (2025).”
Troye Sivan wore it on stage during Charli XCX’s Coachella 2025 set, where they performed “Talk Talk” together — a redux of their joint tour last year. He later posted a photo wearing the shirt alongside Lorde, Charli XCX and Billie Eilish, further cementing its status as an iconic fashion moment. Other high-profile supporters include Addison Rae, Tilda Swinton, Haider Ackermann, Emma Brooks, bbno$, Lisa Rinna and Camille Charriere — all of whom have proudly shared it on social media. Their posts have helped catapult the shirt into the global spotlight, transforming it into both a fundraiser and a visual rallying cry.
The shirt which sells for £75 (about $99 USD), is available through Ives’s website, with 100% of the proceeds benefiting Trans Lifeline — a nonprofit organization run by and for trans people. Since its launch, over 5,000 shirts have been sold, helping to fund Trans Lifeline’s critical services, including its peer-led crisis hotline and its micro-grants program, which has already distributed over a million dollars directly to trans people.
“I think maybe what really sealed the deal for me was reading the quip somewhere where this is a trans-led U.S.-based charity benefiting trans people,” said Ives.
“I’m not the one picking up the phone helping these people or answering the phones. I think that was really why I wanted that to go where it was going,” he emphasized.
He also emphasized the importance of transparency: “When people say $100 for a T-shirt is a lot, we break down the costs for them. We show them how we’re using organic cotton, fair trade environments, reputable factories—and that over two-thirds of proceeds are going to charity.” Ives even encourages critics to take action however they can: “If the shirt isn’t accessible for you, we tell people: make your own, and donate whatever you can directly to Trans Lifeline.”
What started as a closing runway moment has become a movement. “It feels now like it’s turned into something bigger than just a T-shirt,” Ives reflected. “It’s become a universal concept that is for the people as well. We don’t own that phrase.” In fact, when asked about trademarking Protect the Dolls, Ives responded, “Honestly no, because it’s not mine to own.”
“Protect the Dolls” is more than a fashion statement — it’s a declaration of solidarity and a call to action. Every shirt worn is a stand against the forces that seek to erase us, a tangible investment in a future where trans people not only survive, but thrive. It’s a reminder that our lives, our joy, and our futures are worth fighting for.
Because in the face of systemic violence, we protect each other.
We protect the dolls.
Community Perspectives
How a promoter brought Middle East Nights to WeHo Gay Bars
Mas is interested in challenging assumptions in the West about sexuality in the Middle East

Mas never meant to become a club promoter. He’s a broad man with a neat beard and twinkling eyes above a grin. After studying marketing and management in the U.S., he returned to the Middle East to help a Dubai company open luxury movie theaters across the region — including the first ever movie theater in Saudi Arabia.
When Covid-19 hit, theaters shuttered and the Lebanese economy crashed. Banks locked people’s money and so, starting over with nothing, he returned to Los Angeles, where he crashed on a friend’s couch for three months.
Ingenuity makes strange bedfellows. When Micky’s in WeHo offered Mas a bartending gig, he pitched the idea of taking over their marketing campaigns instead. Months later, after helping to get the word out about all sorts of different events and evenings, the club asked him if he’d consider hosting a night.
Mas is interested in challenging assumptions in the West about sexuality in the Middle East by hosting this night in the gay-famous WeHo community.
At the time, Mas says, there were no events for the gay Middle Eastern community in L.A., which includes Arabs, Persians and Armenians. The only other gay, Middle Eastern-oriented club was Club Nur, which is now permanently closed. So he thought of hosting his own.
“I wanted to create a space for us to listen to our music,” said Mas. “A place for us to be homesick.”
As a new promoter, the club didn’t offer Mas a weekend, but rather a Wednesday night, which are notoriously difficult to sell. But the day gave Mas the name for his first foray into nightlife.
“They already call it hump day,” he said.
The associations: camels and being horny.
“Save a Camel, Hump a Habibi,” says the screen at the bar, over an image of a shirtless man surrounded by decorative lamps. “Habibi,” is a word in Arabic without an easy translation. The most direct is, “beloved,” or “my dear,” but the part that defies translation is how it means both “friend” and “lover.”
For the first Hump event, the team brought a real live camel to West Hollywood to stand out in front of Micky’s as a photo op.
“To this day that’s what’s remembered,” he said.
People for the Ethical Treatment of Animals (PETA) got wind of what was happening and was not pleased — but Mas explains with an eye roll, that the camel was there for one hour, on an off night, with two trainers and was well looked after.
Mas then spoke about the club promotion politics of that night.
“I was a closeted college student in Louisiana when 9/11 happened,” he said, sharing how his white American friends ran errands for him in the days following the attacks so he wouldn’t run the risk of harassment just for leaving the apartment.
“I still get searched in every airport,” he laughed.
In 2008, he went on America’s Got Talent to perform belly dancing. During his audition, he told the panel that he was there to show the peaceful side of the Middle East and a producer came to him afterward, thanked him for his bravery, and told him that unfortunately they would have to cut his segment from the show for venturing into politics.
“People assume the West is better for gays, but that’s not always true,” he said. “The first experience of homophobia I remember, coming from Lebanon, was while my family was on vacation in Italy.”
“There were five gay clubs in Lebanon growing up,” said Mas. “They were more hidden than here, but they were there.”
He recalls that in Dubai, gay parties happened all the time, but the addresses would be released last-minute to prevent them from being shut down — much like LA’s thriving queer warehouse party scene. People will always find a way.
“In Lebanon, growing up, there was not one type of music.” Lebanon is a crossroads of culture, and influences from Europe and the Middle East mingled freely. “You’d hear English, Spanish, French, and Turkish, even just in how people greeted each other in the street.”
The mix of tunes at Hump parties reflects this vibrant music scene.
I attended Hump at Chapel at The Abbey in March, and the Persian holiday of Nowruz, the new year and start of spring.
“Tonight we’re celebrating the Persian people,” said Mas enthusiastically.
His framework is based on the question: who is being celebrated?
It’s a mixed crowd, and the music oscillates between American pop hits and Persian pop classics. “This one has 3 million Shazams,” exclaimed the similarly clueless white boy next to me when we look up the song that’s playing — which has inspired an eruption of passionate singing-along from the middle of the dance floor. My friend Ruben, who’s from Guatemala, twirls another man through classic Salsa steps, to the Persian beat.
“I don’t know a word, but it still makes me move my hips,” he laughed.
I was pleasantly surprised to find another friend, Ameed, working at the door. His social media feed is a continual anguished cry for his native Palestine, but here he sports a broad grin under his keffiyeh, welcoming people in.
“I never thought something like this could exist,” he said. “I was nervous my first time coming,” Ameed explains how coming out as gay to his family led him to take a step back from his own culture, even to see it as bad or bullying. “Every gay Arab guy has some sort of trauma,” he says. “But here I get to enjoy the parts of my culture I enjoy, while still feeling safe — and I get to meet other people in the same boat.”
When Mas talked about making a space “to be homesick,” I had taken it literally, imagining folks far from where they grew up longing for that homeland. Speaking with Ameed a new meaning dawns on me — the way we are homesick for parts of ourselves that we lose in coming out, or even just in growing up. West Hollywood nightlife is all about selling a fantasy. The fantasy here is of a self-aware person’s internal multitudes can be, even just for an evening, in harmony.
Sometimes that’s just a fantasy. Ameed, who says he works a boring, normal job, offered to staff the door after his last experience where he complimented a doorman on their keffiyeh, and the doorman didn’t know what he was talking about.
“Oh this? They just told me to put it on,” he said.
It’s always a fine line between celebration and appropriation.
Reflecting on how that night was a model queer utopia, I wonder if there’d be enough actual gogos from the Middle East to staff a night like that. Probably not.
The crowd is out in force by 11pm, but, classic Thursday, starts to thin after midnight. I was surprised by the number of women out, seemingly supporting the gay men in their lives.
While Hump started as a part time endeavor, Mas’s production team now puts on a slew of gay nights at various bars, including Barbearians (think lots of fur and leather, a play on the erotics of “savagery”) as well as, Steam, a bathhouse-themed night in which guests are encouraged to wear only a towel at the bar. While not specifically Middle Eastern, these nights have the fingerprints of their progenitor, from the music played to, at Steam — a Hookah station where guests can smoke water pipes outdoors and send up smoke like the steam at a bathhouse.
These parties have grown, now touring other cities and even bringing a float to WeHo Pride complete with a flying carpet and gay influencers from Iran, Tunisia, and Iraq. Barbearians, now entering its second year, recently hosted its first Mr. Barbearian competition, which will send the winner, Dé Hanno, to represent the event at Mr. International Leather in Chicago. There’s also intercultural collaborations, like Yalla Papi, a Middle Eastern and Latino night that blends the music of both cultures.
“Latinos move their hips side to side, Arabs move them up and down,” said Mas cheekily.
Mas stated that his goal is to foster a sense of cosmopolitanism and inclusivity. Hump and its progeny provide a safe space for queer Middle Eastern men and their allies to express their sexuality, but also create a meeting ground on their “home turf,” that challenges cultural conceptions both internally and externally.
California
Long Beach Pride reaffirms community focus for this year’s festival
This year’s theme is ‘Power of Community’

Long Beach Pride 2025 will take place on May 17 and 18 at Marina Green Park, emphasizing focus on grassroots organizations and local community performers.
“Long Beach Pride has always been more than just a festival—it’s a movement,” said Elsa Martinez, interim president of LB Pride. “This year, more than ever, we’re celebrating the strength, creativity, and unity of our local community.”
Martinez also notes that all the ticket sales directly go toward funding on-the-ground resources.
“As a nonprofit organization, every aspect of the Pride Festival—from ticket sales to vendor partnerships—directly funds our work in the community,” noted Martinez. “This is a festival with purpose.”
As LB Pride amps up for its 42nd annual celebration, the organization has stated that this year marks the return to the roots of Pride. LB Pride stated that they are committed to emphasizing what makes the local community so special and spotlighting local performers, musicians and entertainers.
The organization has also stated that they are committed to ‘justice, inclusion, and the celebration of queer joy.’
“Our strength has always been our solidarity,” said Martinez. “This year’s festival is a reminder of what we can achieve when we lift each other up.”
This year, the main stage will feature a lineup of pop, Hip-hop and Latin talent.
Performers include HYM the Rapper, George Michael Reborn Tribute, Tori Kay, Jewels Drag Show Extravaganza, Secret Service, Tiancho and music mixes by DJ BSelecta, DJ Icy Ice and DJ 360.
For updates, tickets, and volunteer opportunities, please visit https://longbeachpride.com and follow @LongBeachPride on social media.
Commentary
From pride to policy, it’s time to build in WeHo
‘West Hollywood isn’t just coasting on its values—we’re acting on them’

By John M. Erickson, West Hollywood City Councilmember
West Hollywood has always stood as a beacon for LGBTQ people, for the
marginalized—for anyone chasing a place to be safe, seen, and supported. But that
promise is slipping away. If people can’t afford to live here, then West Hollywood becomes a symbol, not a sanctuary.
The housing crisis gripping Southern California is particularly acute in LGBTQ communities. Whether it’s trans women of color pushed into homelessness, queer youth aging out of foster care, or seniors on fixed incomes being priced out of the very neighborhoods they helped shape—our inability to build enough housing is deepening the inequality we claim to fight against. Our failure to build enough housing is not just a policy gap—it’s a moral one.
This isn’t theoretical. It’s personal.
As a gay man and a progressive policymaker, I know what it means to live at the intersection of identity and action. I carry the legacy of those who fought for a seat at the table—and the duty to do more than just sit there. Right now, that means confronting a housing system that’s failing the very people we claim to protect.
When West Hollywood became a city in 1984, we inherited density. We had walkable
neighborhoods, apartment buildings, and a diverse housing stock. But we froze. For 40
years, our zoning has barely moved.
In the last 25 years, WeHo has actually decreased in population. Meanwhile the number
of Americans who identify as LGBTQ+ has more than tripled in that same amount of
time. We haven’t kept up with demand, and we haven’t met the needs of the vulnerable
communities we claim to champion.
That’s about to change.
On Monday, May 5th, I’m introducing a sweeping housing reform package aimed at one
thing: making it easier, faster, and cheaper to build homes in West Hollywood. Not just
luxury condos—homes people can actually live in. That means slashing red tape. Cutting delays. Dismantling outdated rules that stall projects and drive up rents.
This isn’t about bulldozing neighborhoods or silencing community voices. It’s about
fixing a broken system—one built for a different era and completely out of step with the
urgency of now. It’s time to stop confusing progressive branding with progressive
outcomes. We need real reform: faster processes, smarter regulations, and yes—political courage.
Will this fix everything overnight? No. But it will send a clear message: West Hollywood
isn’t just coasting on its values—we’re acting on them.
Housing justice is LGBTQ+ justice. It’s racial justice, economic justice, and generational
justice. We don’t get to call ourselves a queer haven if only the rich and lucky can live
here. The West Hollywood of the future must make room for drag artists, Trader Joe’s
cashiers, trans youth, longtime renters—and anyone else trying to build a life with
dignity.
A city that flies the Pride flag can’t stand by while its most vulnerable residents are
priced out and pushed out. We owe the next generation more than just slogans and
rainbows. Let’s leave them keys.
-

 Breaking News1 day ago
Breaking News1 day agoMajor victory for LGBTQ funding in LA County
-

 Features1 day ago
Features1 day agoKoaty & Sumner: Finding love in the adult industry
-

 a&e features4 days ago
a&e features4 days agoLatina Turner comes to Bring It To Brunch
-

 Books3 days ago
Books3 days agoTwo new books on dining out LGBTQ-style
-

 Television4 days ago
Television4 days ago‘White Lotus,’ ‘Severance,’ ‘Andor’ lead Dorian TV Awards noms
-

 El Salvador1 day ago
El Salvador1 day agoLa marcha LGBTQ+ desafía el silencio en El Salvador
-

 Miscellaneous10 hours ago
Miscellaneous10 hours agoCan you really find true love in LA? Insights from a queer matchmaker
-

 Arts & Entertainment11 hours ago
Arts & Entertainment11 hours agoIntuitive Shana gives us her hot take for July’s tarot reading






