AIDS and HIV
AIDS activists call for urgent meeting with UnitedHealthcare over denial of PrEP
Cited “high risk homosexual sexual behavior”


(Graphic by Troy Masters)
AIDS activists around the country sprang into action after numerous complaints surfaced that at least one insurance carrier—United Healthcare—has been throwing up possibly illegal barriers to accessing the PrEP drug Truvada by people who are HIV positive.
The HIV Healthcare Access Working Group of the Federal AIDS Policy Partnership, which includes APLA Health, sent a letter to United Healthcare Friday, April 4, urging the insurance giant to “reverse the utilization management requirements that took effect July 1, 2017 for Truvada prescribed Pre-Exposure Prophylaxis or PrEP.” This is the story that came to light on Thursday, in which a UHC client was denied his treatment because of his alleged behavior.
“The request for coverage for Truvada is denied. This decision is based on health plan criteria for Truvada. The information sent in shows you are using this medicine for engaging in High risk homosexual behavior,” reads the letter to the HIV patient on Unitedhealthcare letterhead posted on a Facebook site frequented by people impacted by HIV/AIDS. “This determination is considered to be a determination that the requested coverage is not medically necessary under New York State Law for the purposes of your appeal rights.”
“Specifically,” the letter from the advocates for people with HIV/AIDS continues, “we believe requiring detailed documentation to request prior authorization every three months for Truvada prescribed for PrEP and requiring all members to use UHC’s mail-order pharmacy, BriovaRx, violates the Affordable Care Act (ACA)’s non-discrimination protections and federal and state laws barring mandatory mail order policies.”
The HIV policy advocates want to meet with UHC since a number of people have run out of their medications and the hoops UHC now makes patients jump through can take up to two weeks or more.
Lest the insurance carrier misunderstand what harm this policy change can and is doing, the advocates spelled it out for them:
“PrEP is a critical advancement in HIV prevention that, when taken as prescribed, can provide nearly 100% protection from acquiring HIV infection. Stigma and discrimination are major barriers that have impeded uptake of this highly effective prevention intervention. In addition to violating multiple laws, the new policies have been implemented in such a way as to insult and disrespect UHC members. We have been shocked and appalled by the language in the coverage denial letters that are being sent to patients taking Truvada for PrEP and to patients living with HIV taking Truvada as part of a treatment regimen. The denials are contradictory and contain the type of inflammatory and judgmental language that contributes to the stigma that lesbian, gay, bisexual and transgender individuals and others face. In addition to written communications, UHC members have been subject to inappropriate and invasive questioning about their sexual orientation, HIV status and drug use by customer service representatives.”
There have been some scattered reports that UHC has apologized—but it is not posted on their website or their Twitter account. The issue is not simply with the offensive tone of the denial letter but with the July accessibility change in the first place.
“UHC’s Policy Requiring Prior Authorization for PrEP Violates Non-discrimination Protections,” they write. “The federal Medicaid Act and Section 1557 of the ACA prohibit discrimination on the basis of race, color, national origin, disability, age, and sex. Section §1557 prohibits insurance companies that participate in the state exchanges from discrimination based on these characteristics. The sex protections within the ACA have been interpreted to include gender identity, and sex stereotyping which many courts and federal agencies have implemented to also include sexual orientation. These protections extend to discriminatory drug benefit designs, including unjustified prior authorization processes. With specific regard to HIV medications, the court has ruled that placing arbitrary barriers on HIV medications constitutes discriminatory plan design. This applies to PrEP, which is primarily prescribed to gay, bisexual, or same-gender-loving men; black women; or transgender women.”
Additionally, “The mail order requirement is in violation of the 2014 Settlement Agreement arising from John 3 Does I-V v. United Healthcare Insurance Company. The U.S. District Court of the Central District of California ordered United Healthcare to allow their customers taking HIV medications to opt-out of a mail order pharmacy requirement due to concerns about safety and privacy. The plaintiff class was concerned that their HIV status and sexual orientation would be inadvertently disclosed during delivery of their medications. UHC customers taking PrEP share those concerns,” they write.
“Home delivery of medications to individuals in shared living situations or without secure mail receptacles puts UHC members living with stigmatized conditions or at risk for stigmatized conditions at unnecessary risk for stigma and discrimination. Truvada also is prescribed to treat HIV and discovery of the medication and other HIV medications threatens UHC members’ safety and privacy, potentially leaving them at risk for violence and discrimination.”
Read the entire letter below:
August 4, 2017
Stephen J. Hemsley
Chief Executive Officer
David S. Wichmann
Office of the Chief Executive President
UnitedHealth Group
P.O. Box 1459
Minneapolis, MN 55440-1459
Dear Mr. Hemsley and Mr. Wichmann:
We, the undersigned organizations, urge United Healthcare (UHC) to reverse the utilization management requirements that took effect July 1, 2017 for Truvada prescribed for Pre-Exposure Prophylaxis or PrEP.
Specifically, we believe requiring detailed documentation to request prior authorization every three months for Truvada prescribed for PrEP and requiring all members to use UHC’s mail- order pharmacy, BriovaRx, violates the Affordable Care Act (ACA)’s non-discrimination protections and federal and state laws barring mandatory mail order policies. We respectfully request a meeting to discuss the impact of these new policies on UHC customers.
PrEP is a critical advancement in HIV prevention that, when taken as prescribed, can provide nearly 100% protection from acquiring HIV infection. Stigma and discrimination are major barriers that have impeded uptake of this highly effective prevention intervention. In addition to violating multiple laws, the new policies have been implemented in such a way as to insult and disrespect UHC members. We have been shocked and appalled by the language in the coverage denial letters that are being sent to patients taking Truvada for PrEP and to patients living with HIV taking Truvada as part of a treatment regimen. The denials are contradictory and contain the type of inflammatory and judgmental language that contributes to the stigma that lesbian, gay, bisexual and transgender individuals and others face. In addition to written communications, UHC members have been subject to inappropriate and invasive questioning about their sexual orientation, HIV status and drug use by customer service representatives.
Excerpt from an OptumRx Denial letter:
“Your request for coverage for Truvada is denied. This decision is based on health plan criteria for Truvada. The information you sent in shows you are taking this medication for High risk homosexual sexual behavior. This medication is only covered if you have HIV Infection, Post exposure prophylaxis (PEP) to reduce the risk of acquisition from either an occupational or non- occupational known or suspected possible exposure to HIV, Pre-exposure prophylaxis (PrEP) to reduce the risk of sexually acquired HIV-1 infection in adults at high risk or Hepatitis B and meet indications specific criteria. You do not meet any of these criteria.” Read full denial letter here.
We urge you to consider the points outlined below and immediately reverse the prior authorization restrictions implemented in July 2017.
UHC’s Policy Requiring Prior Authorization for PrEP Violates Non-discrimination Protections
The federal Medicaid Act and Section 1557 of the ACA prohibit discrimination on the basis of race, color, national origin, disability, age, and sex. Section §1557 prohibits insurance companies that participate in the state exchanges from discrimination based on these characteristics. The sex protections within the ACA have been interpreted to include gender identity, and sex stereotyping which many courts and federal agencies have implemented to also include sexual orientation. These protections extend to discriminatory drug benefit designs, including unjustified prior authorization processes. With specific regard to HIV medications, the court has ruled that placing arbitrary barriers on HIV medications constitutes discriminatory plan design. This applies to PrEP, which is primarily prescribed to gay, bisexual, or same-gender-loving men; black women; or transgender women.1
UHC’s Prior Authorization Policy Is Restricting Access without Justification
We strongly object to the stringent and overly complex prior authorization documentation that is now required to request coverage of Truvada for PrEP. The medical providers prescribing PrEP are better positioned to determine the clinical appropriateness of PrEP for patients as evidenced by the communications that have occurred regarding this issue and the inappropriate denial letters UHC members have received. If prior authorization is maintained, we urge for the process to be significantly simplified and streamlined and for best practices to be followed. In particular, the approval period should be for 12 months, as is standard practice for medications that are prescribed for an extended period. The three-month cycle puts patients at risk of delays and medication interruptions and creates unnecessary burden to providers and anxiety for UHC members.
In order to protect against HIV acquisition, a patient must have consistent access to PrEP without interruption. Delays caused by UHC’s prior authorization approval put individuals at greater risk for acquiring HIV infection.
From a UHC Member:
“I have been on PrEP for three years and with UHC for the past year. I called in a refill of my Truvada to my local Walgreens on Saturday, July 1, with two pills left from my (1 See. 42 U.S.C § 18116; see also 42 C.F.R § 92.101(b)(2)(i), 45 C.F.R. § 84 (b)(4) (stating that a recipient of federal funding may not use criteria or methods of administration that have the effect of discriminating on the basis of disability. Cases interpreting the Americans with Disability act and Section 504 of Rehabilitation Act of 1973 (as well as implementing regulations) have consistently recognized HIV/AIDS as a qualifying disability) previous month’s prescription. I went to the Walgreens to pick up my prescription where I was told by the pharmacist that United Healthcare was requiring a prior authorization for my Truvada.
I called United Healthcare and they confirmed that a prior authorization was now required for Truvada and that a prior authorization request had already been sent to my doctor. I called the doctor’s office to find out if the prior authorization was approved. The office told me that the authorization was denied and I needed to call UHC to find out why. I then called UHC and asked if I could appeal the denial and I was told that I should call my doctor and have them call United Healthcare to start the appeal.
I called my doctor’s office and told them that I wanted to appeal the denial. The doctor’s office said that they need to ask me a few questions in order for the doctor to write a letter of appeal. I was asked how many men I have had sex with, was I a receptive anal sex partner, have a slept with HIV positive men, and if I had ever done crystal methamphetamine. I told the doctor’s office that I did not feel comfortable answering these questions.
I called United Healthcare and I asked to speak with a supervisor. The supervisor told me that it would take up to 15 days to do an appeal and five days to do a prior authorization once the HIV test was done. I told the supervisor that I was out of my Truvada prescription and I asked for them to cover a five day supply and they refused. I was also told that I would be required to fill my prescription through United Healthcare’s mail- order pharmacy.
This was an incredibly frustrating experience and I hope that United Healthcare addresses the barriers they created in having patients fill their Truvada prescriptions.”
UHC’s Mail Order Pharmacy Requirement Violates Existing Law
UHC is in violation of the ACA, 45 CFR § 156.122(e). The law requires any health plan required to offer Essential Health Benefits to allow enrollees to access prescription drug benefits at in- network retail pharmacies, unless there are specific safety or handling requirements that would preclude use of a retail pharmacy. Since July 1, UHC has repeatedly failed to provide an opt-out process for customers prescribed PrEP.
In addition to violating federal law, a number of states have statutes that bar mandatory usage of mail order. Georgia Code § 33-64-7-2, effective July 1, 2017, prohibits insurance companies that own pharmacy benefit managers from requiring their customers to use a mail order pharmacy.
New York State’s Anti-Mandatory Mail Order Law similarly prohibits pharmacy benefit managers from requiring that patients purchase prescription drugs from a mail order pharmacy or pay an additional co-payment fee when such purchases are not made from a mail order pharmacy.
The mail order requirement is in violation of the 2014 Settlement Agreement arising from John 3 Does I-V v. United Healthcare Insurance Company. The U.S. District Court of the Central District of California ordered United Healthcare to allow their customers taking HIV medications to opt-out of a mail order pharmacy requirement due to concerns about safety and privacy. The plaintiff class was concerned that their HIV status and sexual orientation would be inadvertently disclosed during delivery of their medications. UHC customers taking PrEP share those concerns.
Home delivery of medications to individuals in shared living situations or without secure mail receptacles puts UHC members living with stigmatized conditions or at risk for stigmatized conditions at unnecessary risk for stigma and discrimination. Truvada also is prescribed to treat HIV and discovery of the medication and other HIV medications threatens UHC members’ safety and privacy, potentially leaving them at risk for violence and discrimination.
From a UHC member:
“Since December 2015 I have picked up Truvada at a local retail pharmacy by opting-out of the mail-order requirement and having UHC grant an exception to deliver my meds to this specific pharmacy. Now due to the changes that went into effect 1 July 2017 (which I am still unsure what those changes are), the customer service representatives at UHC tell me that I can no longer opt-out. I repeatedly told them that I have major privacy and security concerns over receiving my PrEP through the mail, and they just now seem to be interested in looking to grant me another exception. I am out of PrEP as of tomorrow, and UHC will be responsible for this outrageous and unacceptable lapse in coverage. I am in school to become a physician and this process is mind-bendingly confusing even for me – I cannot fathom how someone without my level of health literacy could navigate these added barriers. This is an attempt to confuse and intimidate a vulnerable population into forgoing the lifesaving preventive services we deserve.”
Conclusion
In response to these concerns, we urge UHC to:
- Remove the prior authorization requirement for Truvada for PrEP. If a prior authorization process is maintained, it should be significantly streamlined, invasive personal information should be removed, and be approved for a 12-month period.
- Remove the mail-order pharmacy requirement and allow customers to opt-out.
- PrEP is an effective prevention intervention that can help to stop HIV in its tracks. UHC members should not be denied access to this highly effective HIV prevention tool. UHC’s prior authorization process is discriminatory and unnecessarily complicated, and the mail order requirement is illegal. For the reasons stated above we believe these actions are discriminatory in nature and reserve the right to pursue this matter further by filing a complaint with the U.S. Department of Health and Human Services Office for Civil Rights, charging unlawful discrimination under the
- Affordable Care Act’s non-discrimination protections.
We reiterate our request to meet with you immediately to discuss the UHC prior authorization policy for PrEP. We look forward to your response within 10 business days.
To schedule a meeting or to resolve questions regarding this letter, please contact:
Ramon Gardenhire, AIDS Foundation of Chicago, (312) 334-0928 or [email protected]
Benjamin Brooks, Health HIV, (202) 507-4737 or [email protected]
Respectfully,
AIDS Foundation of Chicago
AIDS United
APLA Health
Association of Nurses in AIDS Care
Health HIV
Human Rights Campaign
HIV Medicine Association
National Coalition for LGBT Health
National Alliance of State and Territorial AIDS Directors
New York City’s Lesbian, Gay, Bisexual & Transgender Community Center
Project Inform
The AIDS Institute
San Francisco AIDS Foundation
Treatment Action Group
AIDS and HIV
Researchers announce using gene editing tool, HIV cut out of cells
The team eliminated HIV from cells in a laboratory raising hopes of a cure, but cautioned that for now their work represents proof of concept
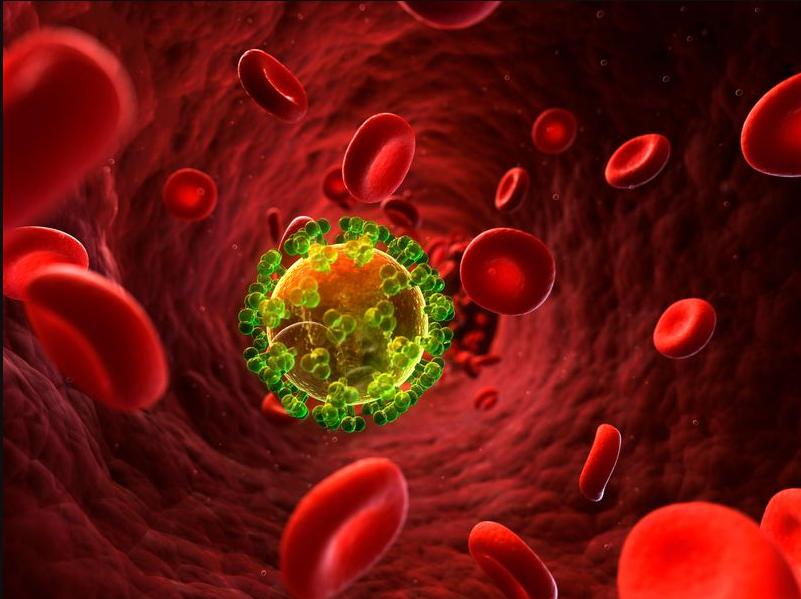
BARCELONA, Spain – Researchers from the Amsterdam University Medical Center made a groundbreaking announcement this week of the results of a major study to be presented at the 2024 European Congress of Clinical Microbiology and Infectious Diseases, which will be held April 27-30 in Barcelona.
A team led by Dr. Elena Herrera-Carrillo using a gene-editing tool known as Crispr-Cas, were able to eliminate HIV DNA, removing all traces of the virus from infected cells. In the press release Tuesday, Dr. Herrera-Carrillo alongside team members Yuanling Bao, Zhenghao Yu and Pascal Kroon, said that utilizing the gene-editing tool they focused on parts of the virus that stay the same across all known HIV strains.
“These findings represent a pivotal advancement towards designing a cure strategy,” the team said.
Herrera-Carrillo’s team works in developing a cure for HIV infection based on novel CRISPR-Cas methods. CRISPR-Cas is a powerful gene editing tool working like genetic scissors but can also be used to selectively attack and inactivate integrated HIV DNA genomes in infected cells.
Herrera-Carrillo’s team eliminated HIV from cells in a laboratory, raising hopes of a cure, but cautioned that for now their work represents proof of concept, and will not become a cure for HIV tomorrow. According to the researchers the next steps involve optimizing the delivery route to target the majority of the HIV reservoir cells within the body.
The hope the research team points out, is to devise a strategy to make this system as safe as possible for future clinical applications, and achieve the right balance between efficacy and safety. “Only then can we consider clinical trials of ‘cure’ in humans to disable the HIV reservoir,” they stated adding, “While these preliminary findings are very encouraging, it is premature to declare that there is a functional HIV cure on the horizon.”
AIDS and HIV
Gilead Sciences awards grants to HIV/AIDS groups in Caribbean, Latin America
Stigma, criminalization laws among barriers to fighting pandemic in region

FOSTER CITY, Calif. — Gilead Sciences this week announced it has given $4 million in grants to 35 organizations in Latin America and the Caribbean that fight HIV/AIDS.
A press release notes Asociación Panamericana de Mercadeo Social (Pan-American Association of Social Marketing) in Nicaragua, Fundación Genesis (Genesis Foundation) in Panama, Fundación por una Sociedad Empoderada (Foundation for an Empowered Society) in Argentina, Associação Nacional de Travestis e Transexuais (National Association of Travestis and Transsexuals) in Brazil and Caribbean Vulnerable Communities are among the groups that received grants. Gilead notes this funding through its Zeroing In: Ending the HIV Epidemic in Latin America and the Caribbean will “improve access to care, increase health equity and reduce HIV-related stigma for populations most affected by HIV.”
“The HIV prevention and care needs of people throughout Latin America and the Caribbean are incredibly diverse, and each of these programs addresses a unique community challenge,” said Gilead Vice President of Corporate Giving Carmen Villar. “Our grantees are deeply embedded in their communities and best positioned to provide needed HIV care and support services.”
“Their expertise will be essential to achieve the Zeroing In program’s goals of improving access to comprehensive care among priority populations, decreasing HIV-related stigma and reducing HIV and broader health inequities,” she added.
The pandemic disproportionately affects Transgender people and sex workers, among other groups, in the region. Activists and HIV/AIDS service providers in the region with whom the Washington Blade has previously spoken say discrimination, stigma, poverty, a lack of access to health care and criminalization laws are among the myriad challenges they face.
First Lady Jill Biden in 2022 during a trip to Panama announced the U.S. will provide an additional $80.9 million in the fight against HIV/AIDS in Latin America through the President’s Emergency Plan for AIDS Relief.
Cuba in 2015 became the first country in the world to eliminate mother-to-child transmission of HIV. The Cuban government until 1993 forcibly quarantined people with HIV/AIDS in state-run sanitaria.
Antigua and Barbuda, St. Kitts and Nevis, Barbados and Trinidad and Tobago in recent years have decriminalized consensual same-sex sexual relations.
The Inter-American Commission on Human Rights in 2021 ruled Jamaica must repeal its colonial-era sodomy law. The country’s Supreme Court last year ruled against a gay man who challenged it.
AIDS and HIV
Local, national events to mark 35th annual World AIDS Day
HIV disproportionately affects certain populations. Men who have sex with men accounted for 70% of 32,100 estimated new HIV infections

WASHINGTON – UNAIDS dubbed this year’s World AIDS Day theme as “Let Communities Lead.” This is how conversations around HIV and AIDS should be structured, Duante’ Brown said, who manages two programs at NMAC — a nonprofit dedicated to working to end the AIDS epidemic. People living with HIV need to be considered the subject matter experts, he said.
“Bringing those people into the room, showing them that they have a voice and that there’s not just this group of people who are making a decision for them … is definitely the way that you go about this.”
Brown manages the ESCALATE program at NMAC, which aims to empower people to address HIV stigma, and the ELEVATE program, which is a training program for people with HIV to be more involved in the planning and delivery of the Ryan White HIV/AIDS Program, which is the largest federal program designed specifically for people with HIV.
In the United States, it’s estimated 1.2 million people are living with HIV, according to HIV.gov. About 13% are unaware they have HIV.
HIV also continues to disproportionately affect certain populations. Men who have sex with men accounted for 70% of the 32,100 estimated new HIV infections in 2021. And Black individuals accounted for 40% of the new infections that year, while only comprising 12% of the population of the United States, according to the CDC.
In 2023, stigma is a key inhibitor to ending the epidemic, Brown said. When stigma gets out of the way, there could be a day when there are no new cases of HIV transmissions, he said. To get around that stigma, people need to have meaningful and productive conversations about AIDS.
“Not treating it as taboo, making sure that we are empowering people living with HIV and AIDS to tell their stories and to be empowered to feel that it’s OK,” Brown said. “And that nothing is wrong with you.”
And there are events in the locally and nationally to recognize World AIDS Day, many of them aimed at abolishing the stigma that comes with talking about HIV.

At a national level, Janet Jackson is set to headline the World AIDS Day concert on Dec. 1 — an annual fundraiser sponsored by the AIDS Healthcare Foundation. The concert will be at the NRG Arena in Houston, and will also honor actor and activist Blair Underwood with its lifetime achievement award.
“[The concert] really is a way to commemorate World AIDS Day in a way that is both remembrance of those that we’ve lost, recognizing where we’re at, but also really celebrating and connecting the work that’s yet to be done. And having folks still leaving uplifted and elevated about what the future could hold,” said Imara Canady, AHF’s national director for communications and community engagement.
Jackson has long been an outspoken advocate for people living with HIV. Her song, “Together Again,” is a tribute to a friend she lost to AIDS, as well as a dedication to patients around the world.
The AIDS Healthcare Foundation, the largest nonprofit HIV/AIDS service organization and advocacy group, has several health care centers in the region and many across the nation and world. AHF also has a free HIV test locater online at freehivtest.net.
AIDSWatch, the electronic memorial to people lost to HIV and AIDS, will be viewable on www.AIDSWatch.org and on the City of West Hollywood’s WeHoTV broadcast and streaming channels, including Spectrum Channel 10 within West Hollywood, beginning at 12:01 a.m. on Thursday, Dec. 1, for 24 hours.
The City of West Hollywood will join STORIES: The AIDS Monument and APLA Health in a World AIDS Day event on Friday, Dec. 1. The evening will begin at 5:30 p.m. with a reception at the West Hollywood Park Aquatic and Recreation Center (ARC) Respite Deck, located at 8750 El Tovar Place.
After a short program with refreshments, attendees will descend the grand staircase of the ARC at 6:30 p.m. in a candlelight procession through West Hollywood Park and along N. Robertson, Santa Monica, and N. San Vicente Boulevards to the City’s Council Chambers/Public Meeting Room, located at 625 N. San Vicente Boulevard. There, the evening will continue with a screening of the award-winning 2023 documentary “Commitment to Life.” Doors will open at 7 p.m. and the screening will begin promptly at 7:15 p.m.
Events are free to attend and open to the public. Limited validated parking will be available at the West Hollywood Park 5-Story structure.
Advance RSVP is requested by reserving a spot on Eventbrite.
AIDS and HIV
Maxine Waters criticizes House GOP over proposed cuts to HIV/AIDS programs
Calif. Democrat spoke at U.S. Conference on HIV/AIDS in D.C.

WASHINGTON — U.S. Rep. Maxine Waters (D-Calif.) on Wednesday sharply criticized House Republicans over their proposed cuts to HIV/AIDS prevention programs.
The California Democrat who represents the state’s 43rd Congressional District in a speech she delivered at the U.S. Conference on HIV/AIDS noted the House Appropriations Committee’s Fiscal Year 2024 Labor, Health, Human Services, Education and Related Agencies Appropriations Bill would cut $767 million from domestic HIV/AIDS programs.
Waters said the bill would cut funds to fight HIV/AIDS among underrepresented groups by 53 percent and “completely eliminates” funding for “Minority AIDS Initiative activities within the Substance Abuse and Mental Health Services Administration.” Waters also noted the appropriations measure “eliminates funding” for the Centers for Disease Control and Prevention’s Ending the HIV Epidemic Initiative, the Ryan White HIV/AIDS Program and community health centers.
“The cuts to the Minority AIDS Initiative will exacerbate racial disparities and the elimination of the (Ending the) HIV Epidemic Initiative,” said Waters.
Waters also criticized House Republicans for “refusing to authorize” the President’s Emergency Plan for AIDS Relief.” The California Democrat said ending PEPFAR “would endanger the lives of millions of people around the world who are living with HIV and endanger the lives of millions more who are at risk.”
“Moreover, it would compromise United States leadership on global health issues,” added Waters. “These programs used to have widespread support. It’s shameful that House Republicans are now trying to eliminate them. We cannot allow these cuts to pass. We cannot compromise. We will not give up.”
U.S. Reps. Jim Jordan (R-Ohio) and Marjorie Taylor Greene (R-Ga.) are among those who Waters criticized by name in her speech.
“I will speak truth to power. I want to use words that they will understand. Hell no! We won’t go! We are not going to give up,” said Waters. “That’s the people’s money. You can’t decide who you’re going to spend it on and not who you’re going to spend it on.”
More than 3,000 people are expected to attend the National Minority AIDS Council-organized conference that will end on Saturday. This year’s theme is “A Love Letter to Black Women.”
“We need a love letter to Black women,” said Waters. “We need it not only from this conference. We need it from our families often times. We need it from our communities. We need it from the churches that we give so much attention to and give our resources to and don’t really get it back. We need a love letter coming from all over this country for what we have suffered, for what we have endured, for the way that we have been denied and for the way that we have been ostracized.”
Waters in her speech specifically praised former Massachusetts Congressman Barney Frank and the late U.S. Sen. Ted Kennedy (D-Mass.) for their work in support of LGBTQ+ rights and efforts to combat HIV/AIDS. Waters also thanked Jewel Thais-Williams, who opened Catch One, a bar and restaurant on Pico Boulevard in Los Angeles that became a refuge for people with HIV/AIDS.
“They had nowhere to gather, nowhere to go, nowhere to be recognized as people who needed support,” said Waters.
B. Kaye Hayes, deputy assistant secretary for infectious disease in the Office of the Assistant Secretary for Health who is also the executive director of the Presidential Advisory Council on HIV/AIDS, is among those who are expected to speak at the conference. Mark S. King, an HIV/AIDS activist and blogger who published “My Fabulous Disease: Chronicles of a Gay Survivor” on Sept. 1, is scheduled to talk on Thursday.
Cal Benn contributed to this story.
AIDS and HIV
American Red Cross ends ban on blood donations by gay men
Many healthy individuals who previously could not give will now be able to support their community through the gift of blood donation

WASHINGTON – The American Red Cross announced a historic change in the organization’s policies regarding blood donations by gay and bisexual men. Under this new donor screening process, all donors answer the same eligibility questions regardless of gender or sexual orientation and will be assessed for blood donation based on individual risk factors, not on sexual orientation.
This change by the Red Cross falls within the U.S. Food and Drug Administration finalized guidelines for blood donation issued this past May that will use a uniform individualized risk assessment questionnaire for respondents regardless of their sexual orientation, sex, or gender.
In a statement the Red Cross noted:
“This change means many healthy individuals who previously could not give will now be able to support their community through the gift of blood donation.
Andrew Goldstein, a cancer researcher from Los Angeles, was a regular blood donor in his younger years before the FDA’s previous policies made him ineligible to donate as a gay man. His desire to influence change compelled him to register as a participant in the FDA funded ADVANCE Study in 2021, which sought to gather data to evaluate the possibility of moving to an individual donor assessment. He is proud he was able to be part of the study that led to this change and is excited to finally be able to give blood again.
“There’s so much in the world that you can’t help with, and you sometimes have to see people going through difficult times, but something like giving blood feels like something so small that you can do, and it means a lot to me that I’ll be able to do that again,” said Andrew. Now, Andrew and many others are able to share their good health with patients in need of lifesaving transfusions.”
The FDA’s new protocols issued in May note that prospective donors who have had a new sexual partner, or more than one sexual partner in the past three months, and anal sex in the past three months, would be ineligible.
So would those who are “taking medications to treat or prevent HIV infection (e.g., antiretroviral therapy (ART), pre-exposure prophylaxis (PrEP) and post-exposure prophylaxis (PEP),” because these drugs can delay the detection of HIV.
Blood donation rules have changed to be more inclusive! All donors will answer the same eligibility questions regardless of gender or sexual orientation, and more people can give lifesaving blood with the Red Cross while keeping the blood supply safe.
— American Red Cross (@RedCross) August 7, 2023
We’ve worked for years… pic.twitter.com/htnLg3AHOm
Related:
AIDS and HIV
Elton John AIDS Foundation launches ambitious new initiative
Throughout Pride Month, Sir Elton John and the co-chairs of The Rocket Fund are challenging supporters to let their #InnerElton out

NEW YORK – The Rocket Fund is the Elton John AIDS Foundation’s latest transformative $125 million campaign to redouble the fight against AIDS everywhere. Growing levels of stigmatization, marginalization, and poverty have led to high rates of HIV and low access to healthcare globally.
“For years, HIV/AIDS has caused enormous pain across the world, but I pray that soon this epidemic will be a thing of the past” said Sir Elton John. “More than 30 years after I launched the Elton John AIDS Foundation, my passion for reaching everyone, everywhere with education and compassionate care is still as strong as ever. The Rocket Fund will turbo-charge our mission and reach those most at risk from this terrible disease. Now is the time. This epidemic has gone on too long. We must all act together to see AIDS defeated in our lifetimes.”
Money from the fund will go towards supporting access to HIV prevention and treatment services, including providing access to HIV tests, antiretroviral therapies, and Pre-Exposure Prophylaxis (PrEP), according to the press release. Donatella Versace, one of the Rocket Fund’s co-chairs — alongside Furnish, Tani Austin, and David Geffen — has also pledged to match donations to the fund up to $300,000 during the month of June.
Throughout Pride Month, Sir Elton John and the co-chairs of The Rocket Fund are challenging supporters to let their #InnerElton out. Letting your #InnerElton out is about proudly expressing your authentic self, showing love for others and taking compassionate action. Supporters are encouraged to join the movement by posting photos of themselves on social media wearing their own take on Elton’s signature looks – or whatever makes them feel their true self – with the hashtag #InnerElton. Many notables are joining to let their #InnerElton out, including Dolly Parton, Michaela Jaé Rodriguez, JoJo Siwa, Heidi Klum, Smokey Robinson and more. Learn more here. The Let Your Inner Elton Out campaign was created by advertising agency Invisible Man and produced in partnership with global communications agency BCW.
The Foundation launched this critical initiative on June 5, the day in 1981 when the Centers for Disease Control released its first report on what would become the AIDS epidemic. This inaugural Rocket Day commemorates the early days of the fight against HIV/AIDS, while committing to accelerate progress towards ending AIDS for all.
“The end of the HIV/AIDS epidemic is within sight, and The Rocket Fund is the push we need to finally cross the horizon,” said David Furnish, Chairman of the Elton John AIDS Foundation. “To end AIDS, we must make targeted investments that can level the playing field, by tackling the inequalities and stigma that prevent people from accessing the care they desperately need. By joining The Rocket Fund and our mission, you can help transform the future for millions of people globally.”
“As we’ve learned through the global fight to stop COVID-19, epidemics do not recognize state borders, economic or cultural differences. If left unchecked, they only worsen with devastating impacts on the most vulnerable,” said Anne Aslett, Chief Executive Officer of the Elton John AIDS Foundation. “It is critical that we meet this moment to connect vulnerable people with the care and resources they need to live vibrant, healthy lives and we welcome all who want to see an end to this disease to join us.”
AIDS and HIV
New data shows HIV infections dropped- mostly among whites
Significant decline in new HIV infections, but impact of prevention efforts far less substantial for Black and Hispanic-Latino populations

ATLANTA – Data published Tuesday. by the Centers for Disease Control and Prevention shows a significant decline in new HIV infections, but suggests the impact of prevention efforts was far less substantial for Black and Latino populations.
From 2017 to 2021, as rates of HIV testing, treatment, and the use of pre-exposure prophylaxis (PrEP) medication rose, new cases dropped by 12 percent overall and by as much as 34 percent among gay and bisexual males aged 13 to 24.
The numbers show a “move in the right direction,” CDC Director Rochelle Walensky said in a press release.
However, when broken down by race, the CDC found new infections were down by 27 percent and 36 percent, respectively, among Black and Hispanic-Latino populations, compared with 45 percent of whites.
Similarly, by 2021 about one third of those who are considered eligible were taking PrEP for HIV prevention, but the CDC noted this number includes “relatively few Black people or Hispanic/Latino people” despite the significant increase in prescriptions up from just 13 percent in 2017.
“Longstanding factors, such as systemic inequities, social and economic marginalization and residential segregation,” Walensky noted, continue to act as barriers “between highly effective HIV treatment and prevention and people who could benefit from them.”
She added, “Efforts must be accelerated and strengthened for progress to reach all groups faster and equitably.”
Robyn Neblett Fanfair, acting director of the CDC’s Division of HIV Prevention, said that “At least three people in the U.S. get HIV every hour—at a time when we have more effective prevention and treatment options than ever before.”
“These tools must reach deep into communities and be delivered faster to expand progress from some groups to all groups,” she said.
The HIV+Hepatitis Policy Institute issued a press release following the CDC’s announcement of the new data, noting both the encouraging progress and need for improvement.
“It appears that our investments in HIV prevention are providing some positive results, but the persistent high number of new diagnoses and the low usage of PrEP among the communities most impacted by HIV point to the need for increased resources, particularly for a national PrEP program,” said the group’s executive director, Carl Schmid.
President Joe Biden’s FY24 budget requested $237 million for a national PrEP program along with $850 million to support the U.S. Department of Health and Human Services’ “Ending the HIV Epidemic in the U.S.” initiative.
AIDS and HIV
President’s Emergency Plan for AIDS Relief marks year 20
Achievements PEPFAR have been remarkable, well-documented by outside evaluators, and hugely applauded throughout the advocacy community

WASHINGTON – The President’s Emergency Plan for AIDS Relief (PEPFAR) marks its twenty year anniversary today, marking the largest commitment by any nation to address a single disease in the world.
The initiative which was personally led and launched by former President George W. Bush in 2003, its funding has totaled more than $110 billion to date, including funding for the Global Fund to Fight AIDS, Tuberculosis and Malaria (Global Fund), to which the U.S. government is the largest donor.
PEPFAR is credited with saving millions of lives and helping to change the trajectory of the global HIV epidemic. The White House today released a statement by President Joe Biden marking the 20th Anniversary:
Twenty years ago today, President George W. Bush declared that preventing and treating HIV/AIDS was a foreign policy priority of the United States. At a time when nearly 30 million people were HIV positive, but very few were receiving life-saving medicines, the President’s Emergency Plan for AIDS Relief (PEPFAR) transformed the global AIDS response and laid a marker for America’s commitment to countries that were impacted the hardest by the AIDS epidemic. Helping lead the bipartisan effort in Congress to authorize PEPFAR is among my proudest achievements from my time in the Senate. To this day, PEPFAR remains a powerful example of America’s unmatched ability to drive progress and make life better for people around the world.
Since 2003, PEPFAR has saved more than 25 million lives and dramatically improved health outcomes in more than 55 partner countries. AIDS-related deaths have declined by 68 percent since their peak in 2004, and new HIV infections are down 42 percent. PEPFAR investments have ensured that 5.5 million babies have been born HIV-free. And two decades of investment in partner nations’ health systems played a critical role in countries’ ability to respond to other health crises such as COVID-19, Mpox, and Ebola.
Today, PEPFAR continues to support 20.1 million people around the world with HIV/AIDS treatment, and my Administration is committed to continuing to lead the global HIV/AIDS response. We will build on our decades of progress to reach the Sustainable Development Goal of ending AIDS by 2030, work to eliminate the stigma and inequities that keep people from accessing care, and keep the voices of people living with HIV/AIDS at the center of our response. I look forward to working with Congress on PEPFAR’s reauthorization this year.
PEPFAR is overseen by the U.S. Global AIDS Coordinator, who is appointed by the President, confirmed by the Senate, and reports directly to the Secretary of State, as established through PEPFAR’s authorizing legislation.
PEPFAR’s original authorization established new structures and authorities, consolidating all U.S. bilateral and multilateral activities and funding for global HIV/AIDS. Several U.S. agencies, host country governments, and other organizations are involved in implementation.
Dr. John Nkengasong, the current coordinator was sworn in on June 13, 2022, and holds the rank of Ambassador leading the Office of the Global AIDS Coordinator (OGAC) at the U.S. Department of State.
Twenty years ago this month, President George W. Bush announced #PEPFAR during his State of the Union address. Since then, the U.S. government has invested $100B+ in the global HIV/AIDS response through PEPFAR, saving 25M lives & bringing us closer to #EndAIDS2030. #PEPFAR20 pic.twitter.com/SMAOHWPZ03
— PEPFAR (@PEPFAR) January 11, 2023
Nobel Prize winning scientist Harold Varmus, who served as Director of the National Institutes of Health (NIH) from 1993 to 1999 and currently the Lewis Thomas University Professor of Medicine at Weill Cornell Medicine in New York City, wrote in an article honoring World Aids Day 2013:
[…] “the PEPFAR story must begin with George W. Bush and his wife, Laura, and their interests in AIDS, Africa, and what Bush termed “compassionate conservatism.” According to his 2010 memoir, Decision Points, the two of them developed a serious interest in improving the fate of the people of Africa after reading Alex Haley’s Roots and visiting The Gambia in 1990.3 In 1998, while pondering a run for the U.S. presidency, he discussed Africa with Condoleezza Rice, his future secretary of state; she said that, if elected, working more closely with countries on that continent should be a significant part of his foreign policy. She also told him that HIV/AIDS was a central problem in Africa but that the United States was spending only $500 million per year on global AIDS, with the money spread across six federal agencies, without a clear strategy for curbing the epidemic.”
Key Facts (As provided by Kaiser Health & Family Foundation)
- Although the U.S. has been involved in efforts to address the global AIDS crisis since the mid-1980s, the creation of the President’s Emergency Plan for AIDS Relief (PEPFAR) in 2003 marked a significant increase in funding and attention to the epidemic.
- PEPFAR is the largest commitment by any nation to address a single disease in the world; to date, its funding has totaled more than $110 billion, including funding for the Global Fund to Fight AIDS, Tuberculosis and Malaria (Global Fund), to which the U.S. government is the largest donor. PEPFAR is credited with saving millions of lives and helping to change the trajectory of the global HIV epidemic.
- U.S. funding for PEPFAR grew from $2.2 billion in FY 2004 to $7.0 billion in FY 2022; FY 2022 funding includes $5.4 billion provided for bilateral HIV efforts and $1.6 billion for multilateral efforts ($50 million for UNAIDS and $1.56 billion for the Global Fund).
- As the COVID-19 pandemic continues to have profound effects across the world, PEPFAR has acted to respond to COVID-19 in countries that receive support in order to minimize HIV service disruptions and leverage the program’s capabilities to address COVID-19 more broadly.
- Looking ahead, PEPFAR faces several issues and challenges, including how best to: address the short- and long-term impacts of COVID-19 on PEPFAR and the HIV response; accelerate progress toward epidemic control in the context of flat funding; support and strengthen community-led responses and the sustainability of HIV programs; define its role in global health security and broader health systems strengthening efforts; and continue to coordinate with other key players in the HIV ecosystem, including the Global Fund.
Key Activities and Results (As provided by Kaiser Health & Family Foundation)
PEPFAR activities focus on expanding access to HIV prevention, treatment, and care interventions. These include provision of antiretroviral treatment, pre-exposure prophylaxis, voluntary male circumcision, condoms, and other commodities related to HIV services. In addition, PEPFAR has launched specific initiatives in key strategic areas. For example, in 2015, PEPFAR launched DREAMS, a public-private partnership that aims to reduce HIV infections in adolescent girls and young women.
The latest results reported by PEPFAR indicate that it has:
- supported testing services for 63.4 million people in FY 2021;
- prevented 2.8 million babies from being born with HIV, who would have otherwise been infected;
- provided care for more than 7.1 million orphans and vulnerable children (OVC);
- supported training for nearly 300,000 new health care workers; and
- supported antiretroviral treatment for 18.96 million people.
- In the 15 countries implementing the DREAMS initiative, new diagnoses among adolescent girls and young women have declined with most DREAMS areas (96%) experiencing declines greater than 25% and nearly two-thirds with declines greater than 40%.
The achievements of the PEPFAR program have been remarkable, well-documented by outside evaluators, and hugely applauded throughout the advocacy community and the developing world. In general, milestones have been met, the program has been enlarged (for instance, to include some research on implementation of medical assistance), the roster of PEPFAR countries has grown and spending plans have not been exceeded.
AIDS and HIV
FDA eases blood donation restrictions for gay & bisexual men
The FDA’s proposal would lift the mandatory three-month deferral period for some men who have sex with men

SILVER SPRING, Md. – The U.S. Food and Drug Administration (FDA) introduced a proposed change to its blood donation guidelines on Friday that would ease restrictions for gay and bisexual men.
The FDA notes the proposal, news of which was first reported in November, would bring U.S. policies in alignment with those in place in countries like the U.K. and Canada. The agency is expected to formally adopt the new guidelines after a public comment period.
The move follows criticism from LGBTQ groups and organizations like the American Medical Association (AMA) who have long argued the current policy is homophobic and based on an outdated understanding of the risks associated with blood donation by men who have sex with men.
As the AMA wrote of the current policy: “a man who has protected sex with another man in the three months prior to a blood donation cannot be a donor, but a man or woman who has unprotected sex with multiple partners of the opposite sex over the same time period remains eligible.”
The FDA’s proposal would lift the mandatory three-month deferral period for some men who have sex with men and instead use a “gender-inclusive, individual risk-based questions relevant to HIV risk.”
Potential donors would be asked for information about their sexual history over the past three months. Respondents who indicate they have had sex with one or more new sexual partners would then be asked whether they have had anal sex during this period. Those who answer “yes” would be deferred from blood donation.
Axios noted that as of this morning, about 20 percent of the country’s community blood centers have a one-day supply or less, while the FDA’s broadened eligibility criteria would increase the annual blood supply by two to four percent, citing data from America’s Blood Centers’ daily tracker and the Williams Institute.
U.S. Sen. Tammy Baldwin (D-Wis.) issued a statement celebrating the FDA’s proposal. “As I have long advocated for, this blood donation policy takes a step forward and is better rooted in the most up-to-date science with a focus on individual risk factors, not outdated stigmas that effectively ban gay and bisexual men,” she said.
Baldwin has repeatedly urged the agency to revisit its blood donation policy over the years, including by corralling support from other members of Congress to cosign letters to the FDA in 2014 and 2016, raising the issue again in 2020 as the COVID-19 pandemic exacerbated shortages in the blood supply.
The Congressional LGBTQ+ Equality Caucus also acknowledged the move in a statement by its chair, Rep. Mark Pocan (D-Wis.): “I am glad the FDA is finally moving toward an individual risk-based assessment model, but recognize, based on existing reporting, that many LGBTQI+ people may still be barred from donating,” he said. “I look forward to taking a closer look at the proposed guidelines once they are published and working with the FDA to ensure that any unnecessary barriers are removed.”
Several LGBTQ groups also issued statements celebrating the FDA’s new guidance.
“These changes are 40-plus years in the making, and are a tremendous leap forward toward elevating science over stigma,” said GLAAD President Sarah Kate Ellis. “GLAAD and leading medical experts have long been advocating for guidelines that see and treat LGBTQ people the same as any other person, including as potential donors who want to help others.”
“This new policy removes a decades-long barrier for many in our community – and there is more to do to ensure gay, bisexual and transgender people are no longer unfairly stigmatized when they try to donate blood,” Human Rights Campaign President Kelley Robinson said. “The assessment criteria have flaws, focusing excessively, for instance, on the number of partners a potential donor has instead of just on new partners,” she added.
Carl Schmid, executive director of the HIV+ Hepatitis Policy Institute, said: “While this long-overdue change is being made based on the science and the facts, which have been clear for years, it is the result of the leadership of the Biden administration that continues to tear down discriminatory government policies.”
AIDS and HIV
Experimental HIV vaccine failure, deemed safe but ineffective
“We remain steadfast in our commitment to advancing innovation in HIV & hope the data from Mosaico will provide insights for future efforts”

BETHESDA, Md. – A clinical trial of an investigational HIV vaccine regimen, being conducted in partnership with the National Institute of Allergy and Infectious Diseases (NIAID) by Janssen Pharmaceutical Companies and global partners of parent company Johnson & Johnson dubbed “Mosaico,” was discontinued.
In an announcement made Wednesday, NIAID said the HIV vaccine regimen tested among men who have sex with men (MSM) and transgender people was safe but did not provide protection against HIV acquisition, an independent data and safety monitoring board had determined.
A spokesperson for Johnson & Johnson noted in light of the board’s determination, the Mosaico clinical trial will be discontinued. Participant notifications and further analyses of the data are underway. Throughout the trial, study investigators have ensured that any individuals who contracted HIV received prompt HIV treatment and care.
Both Johnson & Johnson and NIAID stressed that no safety issues with the vaccine regimen were identified.
“We are disappointed with this outcome and stand in solidarity with the people and communities vulnerable to and affected by HIV,” said Penny Heaton, M.D., Global Therapeutic Area Head, Vaccines, Janssen Research & Development, LLC. “Though there have been significant advances in prevention since the beginning of the global epidemic, 1.5 million people acquired HIV in 2021 alone, underscoring the high unmet need for new options and why we have long worked to tackle this global health challenge. We remain steadfast in our commitment to advancing innovation in HIV, and we hope the data from Mosaico will provide insights for future efforts to develop a safe and effective vaccine. We are grateful to our Mosaico partners and the study investigators, staff and participants.”
Janssen Vaccines & Prevention sponsored the Mosaico study with funding support from NIAID, part of the National Institutes of Health. The trial was conducted by the NIAID-funded HIV Vaccine Clinical Trials Network, based at the Fred Hutchinson Cancer Research Center in Seattle. The U.S. Army Medical Research and Development Command provided additional study support.
The Phase 3 Mosaico Study:
Mosaico, a Phase 3 study of Janssen’s investigational HIV vaccine regimen, began in 2019, and completed vaccinations in October 2022. The study included approximately 3,900 cisgender men and transgender people who have sex with cisgender men and/or transgender people, who represent groups and populations vulnerable to HIV, at over 50 trial sites in Argentina, Brazil, Italy, Mexico, Peru, Poland, Puerto Rico, Spain and the United States.
The study evaluated an investigational vaccine regimen containing a mosaic-based adenovirus serotype 26 vector (Ad26.Mos4.HIV) administered during four vaccination visits over one year. A mix of soluble proteins (Clade C/Mosaic gp140, adjuvanted with aluminum phosphate) was also administered at visits three and four.
The Mosaico DSMB analysis, based on the data available to date, indicated that the regimen does not protect against HIV and the study is not expected to meet its primary endpoint. No safety issues with the vaccine regimen were identified. In light of this, the study will be discontinued, and further analyses are underway.
-

 Tennessee2 days ago
Tennessee2 days agoTennessee: Anti-LGBTQ parents can now foster, adopt LGBTQ kids
-
 Ventura County3 days ago
Ventura County3 days ago“Queers in the Valley” Ojai launches & is ready to celebrate Pride
-

 Research/Study3 days ago
Research/Study3 days ago90 percent of trans youth live in states restricting their rights
-

 California Politics3 days ago
California Politics3 days agoRecognizing & celebrating lesbians: Mayor Pro-Tem of El Cerrito
-

 Politics5 days ago
Politics5 days ago600+ national polls shows Biden & Trump are tied
-

 Politics4 days ago
Politics4 days agoSmithsonian staff concerned about future of LGBTQ programming
-

 Music & Concerts4 days ago
Music & Concerts4 days agoHere is the Earth Day anthem we forgot we needed
-

 Maine3 days ago
Maine3 days agoMaine’s Governor Mills signs trans & abortion sanctuary bill into law
-

 Florida4 days ago
Florida4 days agoGov. DeSantis denounces ‘weaponization’ of book challenges
-

 Political commentary & analysis4 days ago
Political commentary & analysis4 days ago20 bills die as Iowa Legislature adjourns-attacks on LGBTQ+ fail











